Medically reviewed by Dr. Priya Prakash (Rheumatologist, board certified) | Last updated: March 20, 2026
What Is Sjogren’s Syndrome? Symptoms, Causes, Diagnosis & Treatment
Sjogren’s syndrome is a chronic autoimmune disease in which the immune system attacks the glands that make moisture, especially the tear and salivary glands. This causes dry eyes and dry mouth, but the disease can also affect the joints, lungs, kidneys, nerves, skin, and other organs. Early diagnosis and ongoing treatment can reduce dryness symptoms, protect the eyes and mouth, and help monitor for whole-body complications.
If you’re searching what is Sjogren’s syndrome, the simplest answer is that it is an autoimmune disease that mainly causes dryness because the body damages moisture-producing glands. Many patients first notice gritty or burning eyes, dry mouth, trouble swallowing dry food, dental problems, swelling of salivary glands, fatigue, or joint pain. A rheumatologist can help confirm the diagnosis and create an individualized Sjogren’s syndrome treatment plan based on dryness severity, lab testing, gland involvement, and whether other organs are affected.
syndrome
Sjogren’s syndrome may occur on its own or alongside another autoimmune disease such as rheumatoid arthritis or lupus. Although dryness is the best-known feature, some patients also develop fatigue, arthritis-like symptoms, neuropathy, lung disease, kidney problems, or other systemic involvement. Because the disease can overlap with medication-related dryness, thyroid disease, fibromyalgia, lupus, rheumatoid arthritis, and other causes of sicca symptoms, getting the diagnosis right matters.
Table of Contents
- What Is Sjogren’s Syndrome? Simple medical definition
- Sjogren’s syndrome at a glance
- Common Sjogren’s syndrome patterns
- Sjogren’s syndrome symptoms (what it feels like)
- Causes & risk factors
- How Sjogren’s syndrome is recognized
- Comorbidities & whole-body impact
- Prognosis (what to expect long-term)
- Understanding Sjogren’s syndrome: complete disease explanation
- Sjogren’s syndrome vs dry eye alone
- Diagnosis: exam, labs, testing
- Treatment: symptom relief + long-term disease control
- Treatment targets (dryness, function, complications)
- Sjogren’s syndrome vs lupus (quick table)
- When to seek urgent care
- Downloadable Sjogren’s symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Sjogren’s Syndrome? Simple Medical Definition
Sjogren’s syndrome is a chronic systemic autoimmune disease characterized by immune attack on the body’s moisture-producing glands, especially the lacrimal and salivary glands. In short, clinically, what is Sjogren’s syndrome? It is an autoimmune exocrine-gland disease that commonly causes dry eyes and dry mouth, but may also cause fatigue, joint and muscle pain, gland swelling, and involvement of organs such as the lungs, kidneys, nerves, and skin.
Sjogren’s Syndrome at a Glance
Dry eyes and dry mouth The two most recognized symptoms often appear first
Autoimmune gland disease Tear and salivary glands are commonly targeted
Can affect other organs Joints, lungs, kidneys, nerves, and skin may be involved
Often causes fatigue Many patients feel ongoing low energy or body aches
Needs long-term monitoring Dryness control alone is not enough when systemic disease is present
Sjogren’s syndrome is more than simple dryness. It is a systemic autoimmune condition with both gland-related and whole-body effects.
Common Sjogren’s Syndrome Patterns
Sjogren’s syndrome can present in more than one way, which is one reason diagnosis may be delayed. Some patients mainly have dry eyes and dry mouth, while others develop prominent fatigue, joint pain, salivary gland swelling, or systemic organ involvement. Clinicians often think about the disease by whether it appears as primary Sjogren’s syndrome or occurs along with another autoimmune disease.
Classic sicca Sjogren’s Dry eyes and dry mouth dominate
Gland-swelling Sjogren’s Parotid or salivary gland swelling stands out
Systemic Sjogren’s Fatigue, joint pain, lung, kidney, or nerve involvement becomes important
Primary Sjogren’s syndrome Occurs on its own without another defined autoimmune disease
Secondary Sjogren’s syndrome Occurs with lupus, rheumatoid arthritis, or another autoimmune condition
Sjogren’s syndrome symptoms (what it feels like)
Typical Sjogren’s syndrome symptoms include dry eyes, dry mouth, fatigue, and joint or muscle pain. Many patients notice burning or gritty eyes, trouble swallowing dry foods, the need to sip water often, mouth sores, dental decay, swollen glands, dry cough, or vaginal dryness. Some people also develop numbness, rash, chest symptoms, kidney-related problems, or other systemic signs depending on which organs are involved.
Eyes • Mouth • Salivary glands • Joints • Skin • Lungs • Kidneys • Nerves • Energy
Autoimmunity
Often female
Tear and saliva
gland injury
Dryness, fatigue
Systemic signs
Confirm Sjogren’s
Protect organs
Wheel shows a simplified pathway: autoimmune gland injury → dryness and systemic symptoms → evaluation and long-term disease control.
Images for patient education
Dry eye symptoms
Dry mouth and glands
Fatigue and joint pain

Causes & risk factors
Sjogren’s syndrome develops because of abnormal immune activation that targets glands and, in some patients, other organs. Genetic susceptibility, immune-system dysregulation, hormonal influences, and environmental triggers are all thought to play a role. The disease is much more common in women, and it may occur alone or together with other autoimmune disorders such as lupus or rheumatoid arthritis.
- Autoimmune attack on tear and salivary glands
- Dry eyes and dry mouth as core sicca symptoms
- Fatigue, joint pain, and gland swelling in many patients
- Possible anti-SSA/Ro and anti-SSB/La antibody positivity
- Can occur alone or with lupus or rheumatoid arthritis
- Can affect lungs, kidneys, nerves, and other organs in some cases
Evidence-based references (guidelines + high-quality sources)
General patient education: NIAMS. Clinical overview: Mayo Clinic. Diagnosis and treatment overview: Mayo Clinic.
How Sjogren’s Syndrome Is Recognized
Sjogren’s syndrome is recognized by the combination of sicca symptoms, physical findings, autoimmune lab testing, and supportive eye or salivary-gland evaluation. Specialists often look for chronic dry eyes, dry mouth, gland swelling, fatigue, joint pain, positive anti-SSA/Ro antibodies, abnormal tear testing, and reduced salivary gland function. The diagnosis can be difficult because dryness is common and may also be caused by medicines, aging, diabetes, infections, radiation, thyroid disease, or other autoimmune conditions.
Chronic dry eyes and dry mouth
Gritty eye discomfort or frequent water sipping
Salivary gland swelling or dental dryness problems
Fatigue, joint pain, or systemic autoimmune clues
Anti-SSA/Ro antibody support in many patients
Abnormal tear, saliva, or gland biopsy findings
Comorbidities & whole-body impact
Sjogren’s syndrome can affect daily life far beyond dryness because it may influence comfort, eating, sleep, speaking, dental health, vision, energy, and whole-body function. Fatigue, recurrent dental issues, corneal irritation, neuropathy, lung disease, kidney problems, and medication side effects can all shape long-term outcomes. Good care requires attention not only to moisture symptoms, but also to systemic disease activity, gland complications, and the small but important lymphoma risk seen in some patients.
- Chronic eye discomfort and corneal surface irritation
- Dental decay, oral discomfort, and swallowing difficulty from dry mouth
- Fatigue and reduced quality of life
- Joint pain or inflammatory overlap symptoms
- Lung, kidney, nerve, or skin involvement in some patients
- Lymphoma risk monitoring in selected higher-risk cases
Prognosis (what to expect long-term)
Many people with Sjogren’s syndrome live long lives with appropriate symptom control and regular follow-up. Even so, the long-term course depends on how severe the dryness is, whether other organs are affected, and whether complications such as recurrent gland swelling or lymphoma risk factors appear. The central goals are to protect the eyes and mouth, reduce fatigue and inflammation, monitor for systemic disease, and preserve long-term quality of life.
Many patients manage dryness well with ongoing treatment and follow-up.
Some patients need closer monitoring because systemic organ involvement develops.
Good control means safer eyes, better oral health, and better long-term function.
Understanding Sjogren’s Syndrome: Complete Disease Explanation
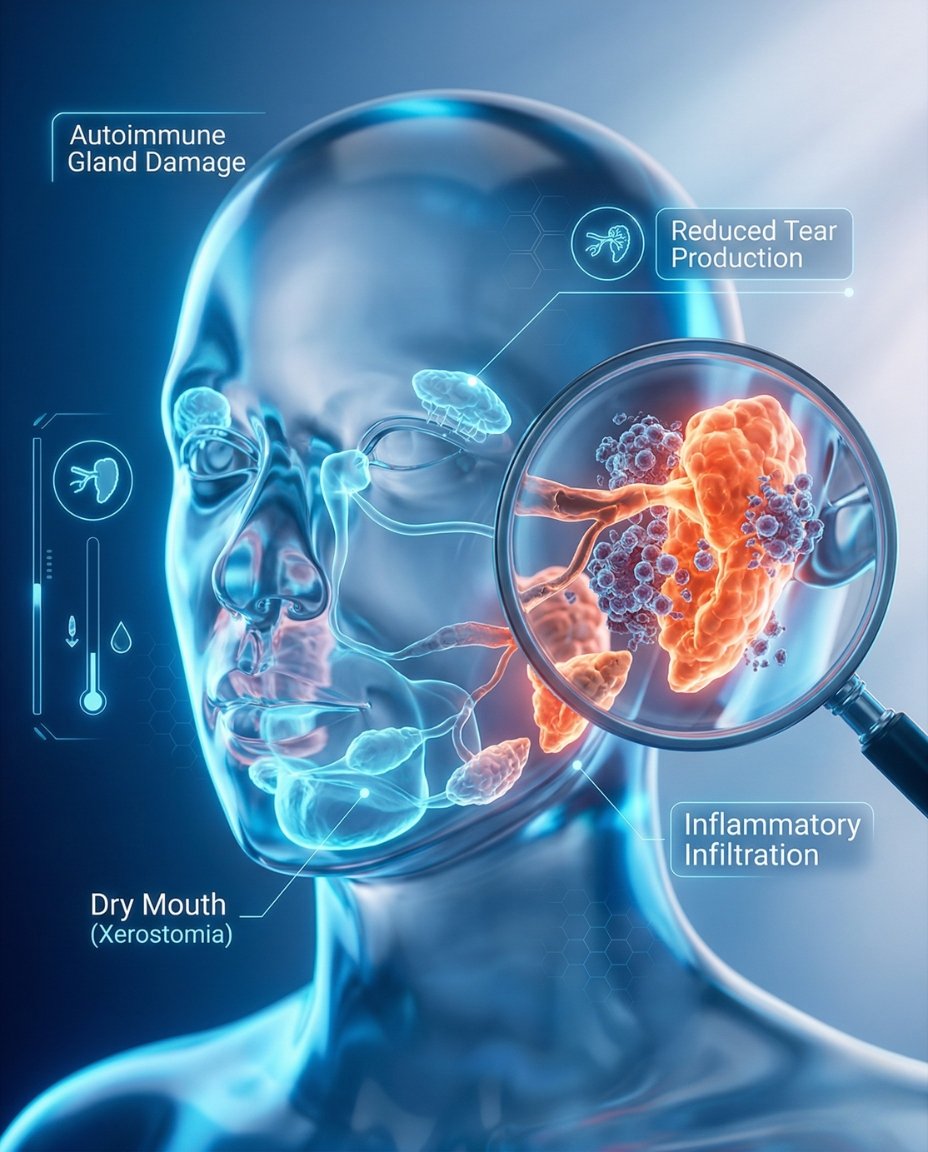
Sjogren’s syndrome occurs when the immune system becomes abnormally activated and attacks glands that normally produce tears and saliva. This helps explain why the eyes and mouth often become dry first, but it also explains how inflammation can extend beyond glands and affect joints, nerves, lungs, kidneys, and other organs. In everyday life, the condition may feel like a dryness problem at first, but in some patients it behaves as a broader systemic autoimmune disease.
What happens at the gland and immune level?
In Sjogren’s syndrome, immune cells infiltrate the moisture-producing glands and reduce normal tear and saliva output. Over time, this can lead to eye irritation, oral dryness, swallowing problems, dental damage, and gland swelling. In some patients, autoimmune inflammation also affects organs beyond the glands, which is why regular monitoring matters even when dryness seems to be the main symptom.
Immune dysregulation → tear and saliva gland inflammation → dryness symptoms → possible systemic involvement of joints, lungs, kidneys, nerves, or skin.
Sjogren’s Syndrome vs dry eye alone
Sjogren’s syndrome and ordinary dry eye are not the same thing, even though both can cause burning or gritty eye symptoms. Sjogren’s syndrome is an autoimmune disease that usually also affects saliva production and may involve fatigue, gland swelling, antibodies, or organ manifestations, while simple dry eye is often more local and non-autoimmune. Distinguishing between them matters because Sjogren’s requires a broader medical evaluation and, in some patients, whole-body monitoring.
Sjogren’s syndrome is a systemic autoimmune disease, not only an eye-surface problem.
Simple dry eye may not involve salivary glands, antibodies, or systemic symptoms.
Correct classification helps guide testing, dental protection, and organ monitoring.
Diagnosis: exam, labs, testing
Sjogren’s syndrome is diagnosed using the overall symptom pattern together with eye testing, salivary gland evaluation, and autoimmune blood work. Doctors may order ANA, anti-SSA/Ro, anti-SSB/La, inflammatory markers, tear tests such as the Schirmer test, salivary flow studies, dental evaluation, imaging, and sometimes a minor salivary gland biopsy. Because not every patient has the same antibody pattern or level of gland damage, diagnosis often depends on combining multiple findings rather than relying on one test alone.
Tests often ordered during initial evaluation
Tests help confirm the diagnosis, define severity, and guide treatment safety.
- Blood tests such as ANA, anti-SSA/Ro, anti-SSB/La, CBC, inflammatory markers, and related autoimmune testing.
- Eye testing such as the Schirmer test and surface staining to measure tear production and eye-surface damage.
- Assessment of dry mouth, salivary flow, dental complications, and gland swelling.
- Imaging or functional salivary-gland testing in selected patients.
- Minor salivary gland biopsy in selected cases when more diagnostic confirmation is needed.
Treatment: symptom relief + long-term disease control
Effective Sjogren’s syndrome treatment has two main goals: relieve dryness symptoms and manage systemic autoimmune disease when present. Many patients use artificial tears, saliva-supportive measures, frequent hydration, dental protection, and other local symptom treatments, while some also need hydroxychloroquine, methotrexate, or other immune-directed therapy depending on the manifestations. Long-term care also includes eye protection, oral care, complication monitoring, and review of organ involvement over time.
1) Symptom control (short-term relief)
Early treatment usually focuses on reducing eye and mouth discomfort and preventing damage from ongoing dryness. Artificial tears, oral moisture strategies, saliva substitutes, and medications that stimulate secretions may help selected patients. Supportive care during this phase may also include antifungal treatment for oral yeast problems, dental prevention, and review of medicines that worsen dryness.
2) Long-term management (disease control and organ protection)
Long-term treatment may include hydroxychloroquine for fatigue, arthralgia, or inflammatory symptoms, and immunosuppressive therapy when systemic organ disease is present. The main goal is to keep symptoms controlled, protect the corneas and teeth, reduce inflammation when needed, and monitor for complications such as lung, kidney, nerve, or lymphoma-related concerns. Long-term care also includes regular dental and eye follow-up, lab monitoring, and reassessment of systemic symptoms over time.
3) Lifestyle strategies that support treatment
- Use regular eye lubrication and follow eye-care guidance to reduce dryness-related irritation and surface damage.
- Sip water regularly, support saliva production as advised, and protect dental health with consistent oral hygiene and checkups.
- Report gland swelling, unexplained weight loss, prolonged fevers, numbness, or persistent cough because these may signal broader disease activity.
- Avoid or review medications that can worsen dryness when possible and medically appropriate.
- Keep follow-up visits because Sjogren’s symptoms and organ involvement can change over time.
Treatment targets (dryness, function, complications)
In Sjogren’s syndrome, treatment targets focus on improving moisture symptoms, protecting the eyes and mouth, and reducing the risk of systemic complications. Clinicians track eye comfort, tear production, swallowing and oral symptoms, fatigue, dental health, gland swelling, lab findings, and any organ-specific disease patterns. Good control means more than less dryness alone; it also means safer vision, better oral function, preserved nutrition, and careful monitoring for systemic disease.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Dryness control | Eye burning, gritty sensation, mouth dryness, swallowing, need for water | Better comfort and less day-to-day sicca burden |
| Function and tissue protection | Vision comfort, oral intake, dental health, gland symptoms, fatigue | Safer eyes, better oral function, and improved daily quality of life |
| Complication monitoring | Organ symptoms, antibody context, gland swelling, nerve or lung signs, lymphoma risk clues | Stable disease with protected organs and earlier recognition of complications |
Case Study 1 (Example)
Patient experienced persistent dry eyes and dry mouth along with fatigue and joint discomfort. Evaluation suggested Sjögren’s syndrome rather than dehydration- symptoms or medication side effects.
Sjogren’s Syndrome vs lupus (quick comparison)
Sjogren’s syndrome and lupus are both autoimmune diseases, and they can overlap, but they are not the same condition. Sjogren’s syndrome centers more on dryness from gland involvement, while lupus is a broader multisystem autoimmune disease with more variable organ inflammation patterns. Distinguishing between them matters because the symptom focus, testing emphasis, and long-term monitoring priorities may differ.
| Feature | Sjogren’s syndrome | Lupus |
|---|---|---|
| Main pattern | Dry eyes, dry mouth, gland dysfunction, fatigue | Multisystem autoimmune inflammation with variable organ involvement |
| Common early clues | Gritty eyes, water sipping, mouth dryness, dental issues | Fatigue, rash, joint pain, photosensitivity, ulcers |
| Typical testing | Tear tests, saliva evaluation, anti-SSA/Ro, biopsy in selected cases | ANA, anti-dsDNA, complements, urine testing, organ-specific evaluation |
| Gland symptoms | Very common and central to diagnosis | Can occur, but are not the main defining feature |
| Treatment focus | Moisture support plus immune treatment when systemic disease is present | Organ protection and immune control based on severity and organ involvement |
When to seek urgent care
- Severe eye pain, sudden vision change, or symptoms suggesting significant corneal injury.
- Marked gland swelling, high fever, rapidly worsening swallowing trouble, or suspected infection.
- Shortness of breath, chest symptoms, numbness, weakness, or other possible organ-related complications.
- Rapid overall worsening, unexplained weight loss, or symptoms that no longer fit a simple dryness pattern.
Call Now for Sjogren’s Syndrome Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My eyes and mouth were always dry, and I was exhausted all the time. The team helped me understand Sjogren’s syndrome and finally connect the symptoms.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Sjogren’s syndrome is a chronic but manageable autoimmune disease that can affect moisture glands, comfort, energy, and in some cases multiple organs. If you have persistent dry eyes, dry mouth, gland swelling, fatigue, or unexplained autoimmune-type symptoms, a rheumatology evaluation can help confirm the diagnosis and build the right long-term treatment plan.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always seek prompt care for severe eye pain, vision change, swallowing difficulty, chest symptoms, or rapidly worsening systemic symptoms.
© 2026 Rheumatology Care Associates. All rights reserved.