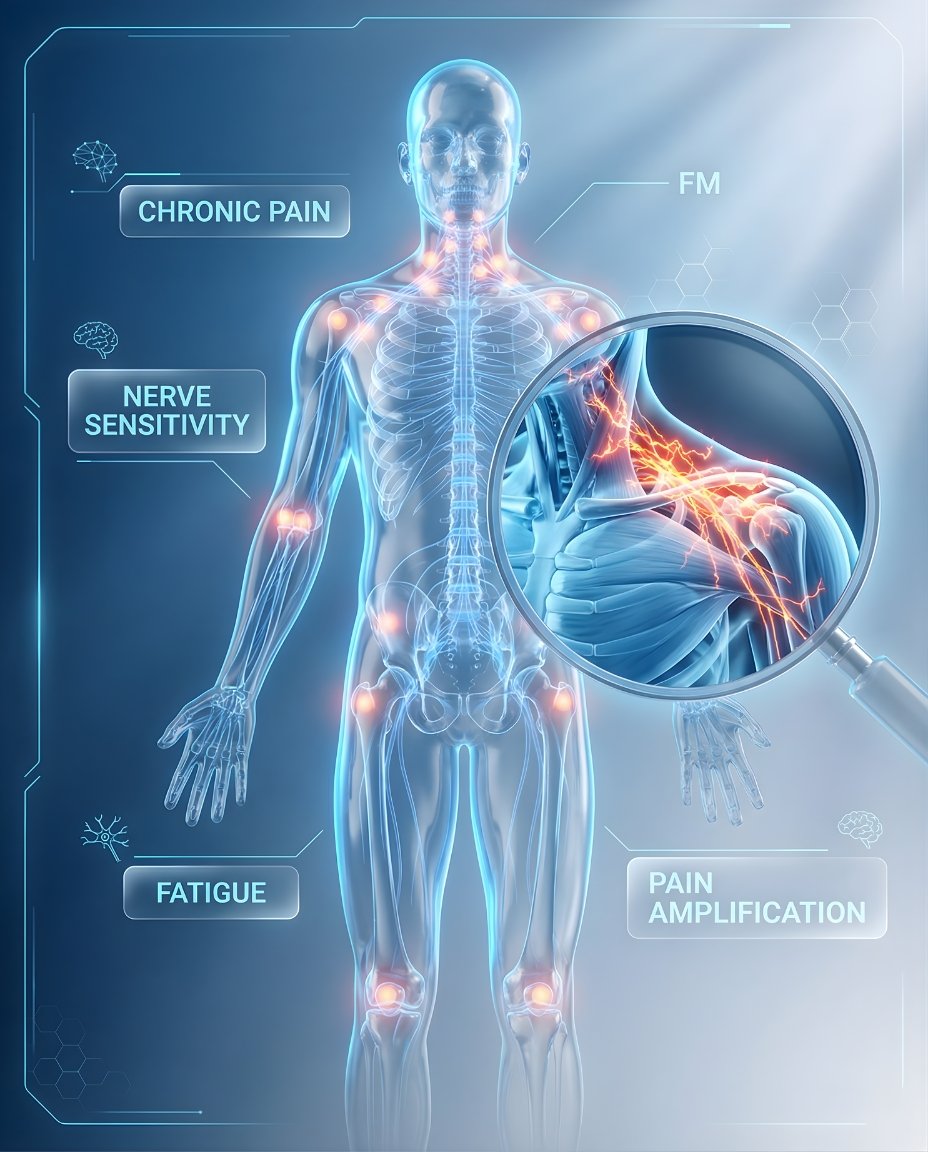
What Is Fibromyalgia (FM)? Symptoms, Causes, Diagnosis & Treatment
Fibromyalgia (FM) is a chronic pain syndrome that causes widespread body pain, fatigue, stiffness, sleep problems, and “fibro fog.” It is not considered an inflammatory or autoimmune arthritis, and routine tests are often normal. Early recognition and a structured treatment plan can improve function, sleep, and day-to-day quality of life.
If you’re searching what is fibromyalgia, the simplest answer is that FM is a long-term pain-processing disorder in which the nervous system becomes more sensitive to pain signals. Many people notice body-wide aching, poor sleep, morning stiffness, low energy, and difficulty thinking clearly. A rheumatologist may help rule out inflammatory disease and identify fibromyalgia, then guide a practical fibromyalgia treatment plan focused on symptom control and function.
Myalgia
Many patients describe pain “all over,” unrefreshing sleep, fatigue, and flare-ups that worsen with stress, overactivity, poor sleep, or illness. FM can also overlap with headaches, anxiety, depression, irritable bowel symptoms, and concentration problems. Because symptoms can mimic inflammatory arthritis or thyroid and other medical conditions, getting the diagnosis right matters.
Table of Contents
- What Is Fibromyalgia? Simple medical definition
- Fibromyalgia at a glance
- Common symptom patterns in fibromyalgia
- Fibromyalgia symptoms (what it feels like)
- Causes & risk factors
- How fibromyalgia is recognized
- Comorbidities & whole-body impact
- Prognosis (what to expect long-term)
- Understanding fibromyalgia: complete disease explanation
- Fibromyalgia vs inflammatory arthritis
- Diagnosis: exam, labs, evaluation
- Treatment: symptom relief + long-term management
- Treatment targets (pain, sleep, function)
- Fibromyalgia vs rheumatoid arthritis (quick table)
- When to seek urgent care
- Downloadable fibromyalgia symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Fibromyalgia? Simple Medical Definition
Fibromyalgia (FM) is a chronic pain syndrome characterized by widespread musculoskeletal pain, fatigue, and sleep disturbance. In short, clinically, what is fibromyalgia? It is a disorder of pain regulation in which the body becomes more sensitive to pain and other sensory input, often causing widespread symptoms even when routine tests are normal.
Fibromyalgia at a Glance
Widespread pain Aching or burning discomfort in multiple body areas
Fatigue Low energy and poor stamina are common
Sleep disturbance Sleep may be unrefreshing even after a full night
Fibro fog Memory and concentration problems may occur
Normal tests Routine labs and imaging are often unrevealing
Symptoms can fluctuate, and flares often worsen after stress, lack of sleep, or too much activity.
Common Symptom Patterns in Fibromyalgia
Fibromyalgia can look different from person to person. Clinicians often think about the balance of pain, fatigue, sleep problems, cognitive symptoms, and overlapping syndromes such as headaches or irritable bowel symptoms.
Pain-dominant pattern Widespread aching and tenderness are the main complaint
Fatigue-dominant pattern Exhaustion and low stamina affect daily life
Sleep-related pattern Poor or unrefreshing sleep drives daytime symptoms
Cognitive pattern Brain fog, memory trouble, or poor focus may stand out
Mixed pattern Pain, fatigue, sleep, and mood symptoms often overlap
Fibromyalgia symptoms (what it feels like)
Typical fibromyalgia symptoms include widespread pain, morning stiffness, fatigue, and poor sleep. Many people also report brain fog, headaches, sensitivity to touch, noise or temperature, and flares after physical or emotional stress. Some patients have associated irritable bowel symptoms, anxiety, depression, or pelvic and bladder discomfort.
Neck • Shoulders • Back • Hips • Arms • Legs • Sleep • Energy • Concentration
Stress
Sleep disruption
Sensitivity
Amplified signals
Pain, fatigue
Brain fog
Rule out mimics
Management plan
Wheel shows a simplified pathway: pain sensitivity → widespread symptoms → evaluation and long-term management.
Images for patient education
Widespread pain
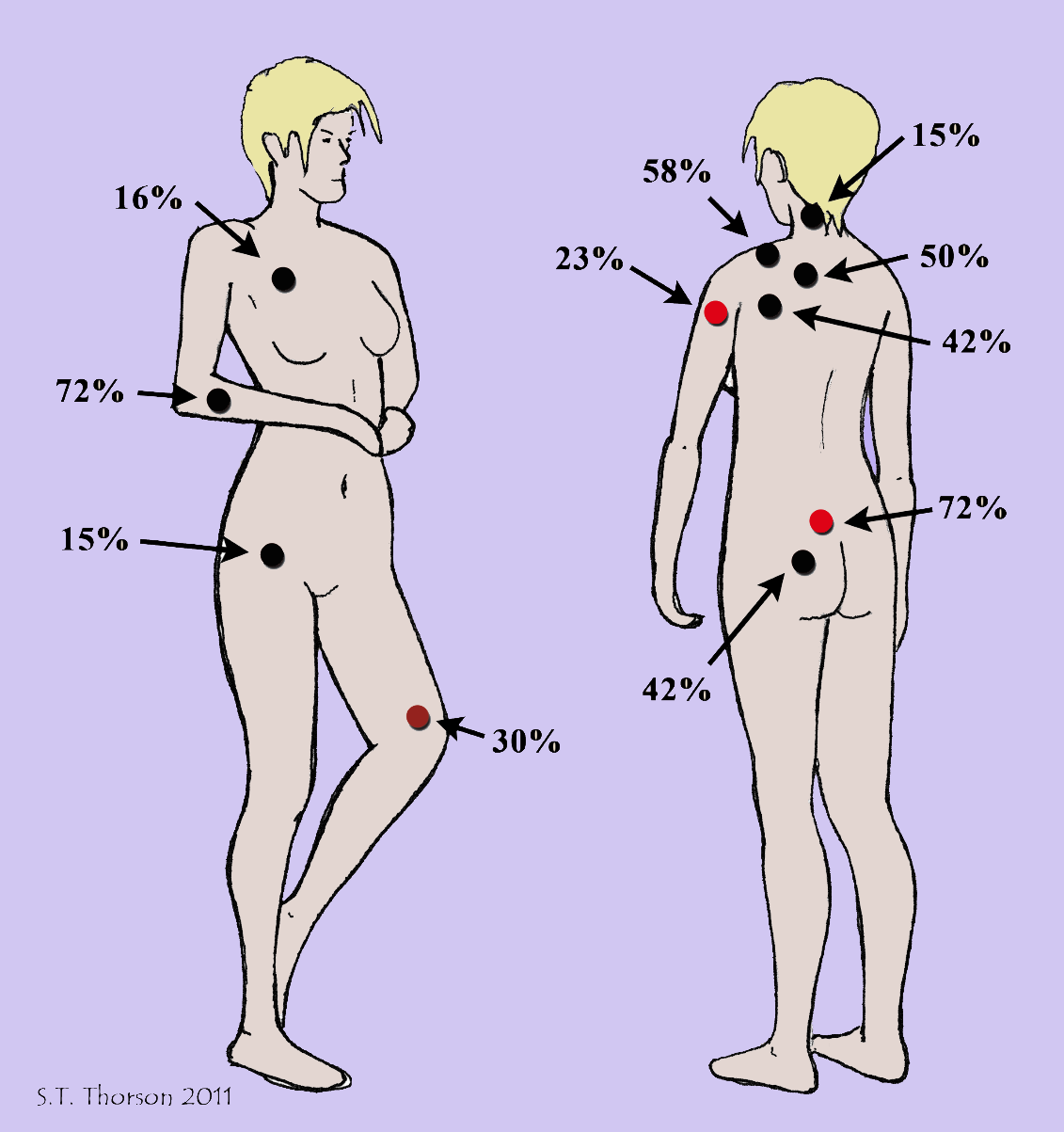
Fatigue and sleep

Fibro fog

Causes & risk factors
Fibromyalgia is not fully understood, but current thinking points to altered pain processing in the nervous system rather than joint inflammation or autoimmune damage.[web:51] Risk may be influenced by poor sleep, physical or emotional stress, mood symptoms, chronic pain conditions, and sometimes illness or trauma preceding symptom onset.[web:51] People with other rheumatic diseases can also have fibromyalgia at the same time, which can complicate symptom interpretation.
- Widespread pain lasting at least several months
- Fatigue and unrefreshing sleep
- Brain fog or poor concentration
- Symptom flares after stress or overactivity
- Normal or near-normal routine tests despite significant symptoms
Evidence-based references (guidelines + high-quality sources)
General patient education: RheumInfo. Fibromyalgia criteria: RheumInfo criteria. Clinical overview: NIH/NCBI StatPearls.
How Fibromyalgia Is Recognized
Fibromyalgia is recognized using the overall symptom pattern rather than one single laboratory or imaging test.[web:52][web:59] Specialists often look for widespread pain lasting at least three months, along with fatigue, sleep disturbance, cognitive symptoms, and the absence of another condition that better explains the full pattern.[web:52][web:59]
Widespread pain in multiple body regions
Fatigue and unrefreshing sleep
Brain fog or concentration difficulty
Symptoms lasting at least three months
No better explanation from another disease
Comorbidities & whole-body impact
Fibromyalgia is not only a pain condition. Many patients also have poor sleep, anxiety, depression, headaches, irritable bowel symptoms, pelvic pain, or urinary symptoms that affect daily quality of life.[web:53][web:55][web:59] High-quality care looks at function, sleep, mood, and activity tolerance in addition to pain intensity alone.
- Unrefreshing sleep and daytime exhaustion
- Brain fog, memory trouble, or poor concentration
- Anxiety or depression symptoms
- Headaches or migraine overlap
- IBS-type digestive symptoms or bladder irritation
- Reduced work, exercise, or daily function during flares
Prognosis (what to expect long-term)
Fibromyalgia is usually a long-term condition, but symptom intensity can rise and fall over time. It does not typically damage joints the way inflammatory arthritis can, but it can strongly affect sleep, stamina, mood, and function if untreated. The goal is to improve symptom control, restore activity, and reduce flare intensity over time.
Symptoms can improve with structured management.
Function often gets better when sleep, pacing, and movement are addressed together.
Many patients need gradual, sustained strategies rather than one quick fix.
Understanding Fibromyalgia: Complete Disease Explanation
Fibromyalgia happens when pain regulation becomes altered, making the body more sensitive to pain and other sensory input.[web:51] Over time, poor sleep, stress, inactivity, and symptom flares can reinforce pain, fatigue, and reduced function. A complete evaluation usually looks at the whole pattern of pain, sleep, thinking, mood, and overlapping symptoms rather than focusing on one body part alone.
What happens at the body level?
In fibromyalgia, the problem is not usually joint destruction or classic inflammation. Instead, the nervous system appears to amplify pain and related symptoms more than expected.[web:51] This helps explain why people may hurt “all over” even when X-rays, scans, or routine blood tests are normal.
Altered pain processing → widespread pain, fatigue, poor sleep, brain fog → chronic symptom cycle without structured management.
Fibromyalgia vs inflammatory arthritis
Fibromyalgia can overlap with inflammatory arthritis, but it is not itself an inflammatory or autoimmune arthritis.[web:53][web:58][web:61] Inflammatory arthritis tends to cause objective joint swelling, inflammatory lab findings, or imaging changes, while fibromyalgia more often causes widespread tenderness, fatigue, and normal routine testing.
The treatment plan for fibromyalgia is different from the treatment plan for autoimmune arthritis. Correct classification helps avoid unnecessary medication and improves focus on exercise, sleep, pacing, and symptom management.[web:59]
Diagnosis: exam, labs, evaluation
Fibromyalgia is diagnosed using the overall pattern: widespread pain, fatigue, poor sleep, cognitive symptoms, and symptom duration, together with evaluation for other explanations.[web:52][web:59] Routine laboratory and imaging tests are often normal, but clinicians may still order selected tests to rule out conditions such as thyroid disease, inflammatory arthritis, or other pain disorders.[web:56][web:59]
Tests often ordered during initial evaluation
Tests help rule out mimics and guide the diagnosis when symptoms overlap with other conditions.[web:56][web:59]
- Basic blood tests to look for thyroid disease, inflammation, or other mimics.[web:56][web:59]
- Symptom-based review using fibromyalgia criteria tools when appropriate.[web:52][web:59]
- Focused physical exam to assess widespread pain and exclude another clear cause.[web:59]
- Additional testing only when the history suggests another diagnosis.[web:59]
Treatment: symptom relief + long-term management
Effective fibromyalgia treatment has two main goals: reduce symptom burden now, and improve long-term sleep, function, and quality of life. Treatment works best as a combined plan using education, pacing, exercise, sleep-focused strategies, and sometimes medication rather than relying on one intervention alone.
1) Symptom control (short-term relief)
Short-term relief may include sleep improvement, activity pacing, stress reduction, and selected medications when needed.[web:59] The best approach depends on the balance of pain, fatigue, mood symptoms, and how much function is affected.
2) Disease control (long-term management)
Long-term management often emphasizes graded exercise, cognitive-behavioral strategies, education, and medications such as duloxetine, milnacipran, pregabalin, or low-dose amitriptyline in selected patients.[web:59] Improvement is usually gradual, so the goal is steady functional recovery rather than a single quick fix.[web:59][web:63]
3) Lifestyle strategies that support treatment
- Use regular low-impact exercise and build activity gradually.
- Protect sleep with a consistent sleep schedule and sleep-hygiene habits.
- Practice pacing so that “good days” do not trigger crashes afterward.
- Address stress, anxiety, or depression because they can worsen symptom severity.
Treatment targets (pain, sleep, function)
In fibromyalgia, treatment targets focus on reducing widespread pain, improving sleep, lowering fatigue, and restoring function. This means clinicians track symptoms, stamina, daily activity, sleep quality, and quality of life over time rather than looking for one lab marker.[web:52][web:59]
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Pain | Widespread aching, tenderness, flare frequency | Lower pain burden and fewer severe flares |
| Sleep and fatigue | Sleep quality, stamina, morning refreshment | Better rest and more energy |
| Function | Daily activity, work, exercise, concentration | Improved participation and consistency |
Case Study 1 (Example)
Patient experienced widespread body pain, fatigue, and sleep disturbances without visible inflammation. Evaluation suggested fibromyalgia rather than joint- arthritis or vitamin deficiency alone.
Fibromyalgia vs rheumatoid arthritis (quick comparison)
Fibromyalgia and rheumatoid arthritis can both cause pain and morning symptoms, but rheumatoid arthritis is an inflammatory autoimmune joint disease while fibromyalgia is a pain-processing disorder. RA is more likely to cause objective joint swelling and inflammatory findings, while fibromyalgia more often causes widespread pain, fatigue, poor sleep, and normal routine tests.
| Feature | Fibromyalgia (FM) | Rheumatoid arthritis (RA) |
|---|---|---|
| Main pattern | Widespread pain, fatigue, poor sleep | Inflammatory joint disease |
| Inflammation | Not typically inflammatory | Inflammatory autoimmune process |
| Tests | Often normal routine labs and imaging | May show inflammatory labs or imaging changes |
| Symptoms | Brain fog, fatigue, widespread tenderness | Swollen painful joints and inflammatory stiffness |
When to seek urgent care
- New chest pain, fainting, major shortness of breath, or other symptoms suggesting a non-fibromyalgia emergency.[web:59]
- Rapid neurologic changes, severe weakness, or symptoms suggesting another diagnosis.[web:59]
- Major depression, panic, or thoughts of self-harm, which need urgent support.
- Sudden major worsening with fever, swollen joints, or other signs that suggest an inflammatory or infectious condition instead.[web:59]
Call Now for Fibromyalgia Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My pain and fatigue were taking over daily life. The team explained what fibromyalgia is and helped me build a plan that finally made sense.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Fibromyalgia is a treatable chronic pain syndrome that often affects sleep, energy, concentration, and daily function in addition to pain.[web:51] If you have widespread pain, poor sleep, fatigue, and brain fog without a clear explanation, a rheumatology evaluation can help rule out inflammatory disease and clarify the next steps.[web:52][web:59]
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always consult with your existing healthcare provider before starting new treatments. Dr. Priya Prakash and Rheumatology Care Associates are committed to evidence-based, personalized care.
© 2026 Rheumatology Care Associates. All rights reserved.