Medically reviewed by Dr. Priya Prakash (Rheumatologist, board certified) | Last updated: March 20, 2026
What Is Bursitis? Symptoms, Causes, Diagnosis & Treatment
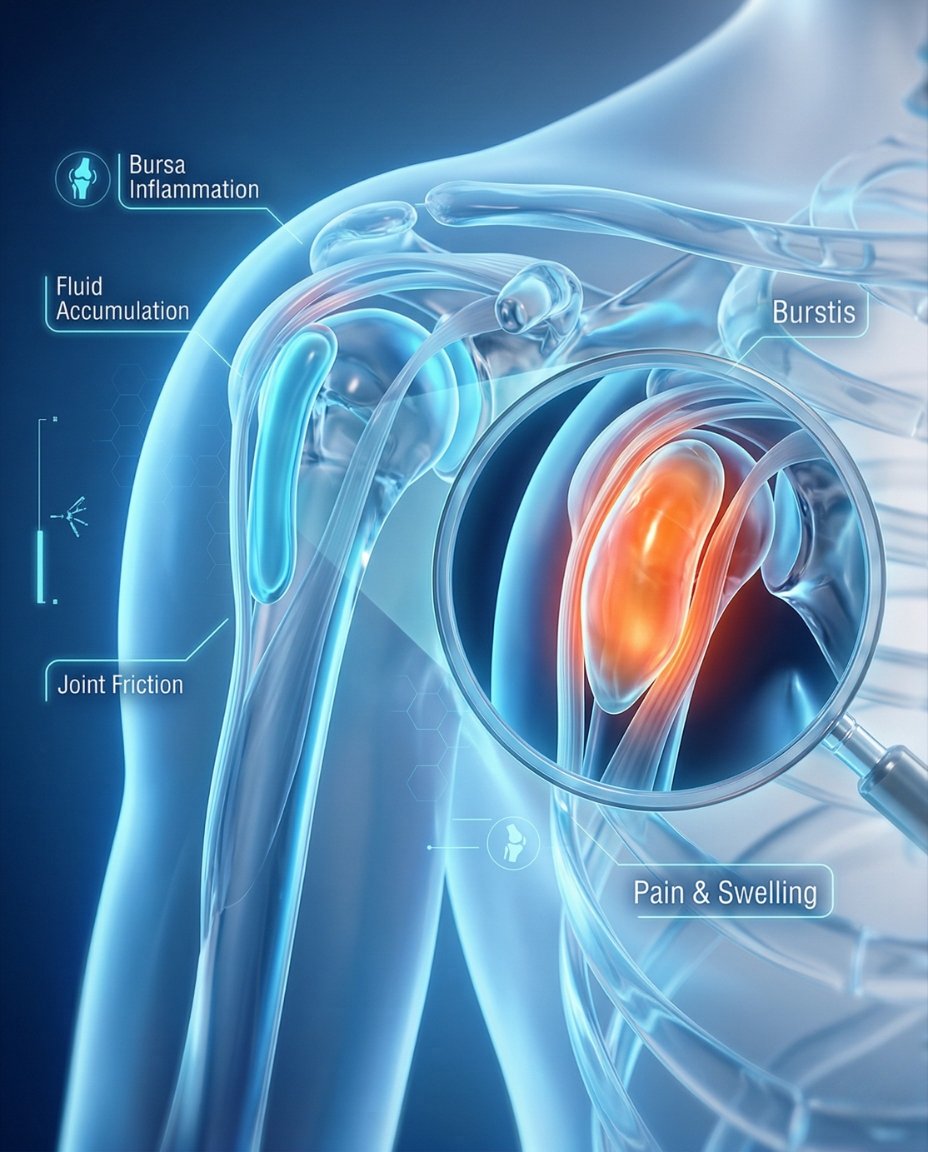
Bursitis is inflammation or irritation of a bursa, a small fluid-filled sac that reduces friction between bones, tendons, and muscles near joints. It commonly causes pain, swelling, tenderness, and limited movement in areas such as the shoulder, elbow, hip, knee, or heel. Most cases improve with rest, ice, activity modification, and other conservative treatment, but some patients need injections, aspiration, antibiotics, or further evaluation depending on the cause.
If you’re searching what is bursitis, the simplest answer is that it is a condition in which one of the body’s cushioning sacs becomes irritated, swollen, and painful. This often happens after repetitive movement, pressure, overuse, injury, or sometimes infection. A rheumatologist, orthopedist, sports medicine physician, or primary care clinician can help confirm the diagnosis and create an individualized bursitis treatment plan based on the location, cause, and severity of symptoms.
Bursitis can occur in many parts of the body, but it is especially common in the shoulder, elbow, hip, knee, and heel. Some cases are short-lived and clearly linked to overuse, while others may be related to infection, gout, inflammatory arthritis, or ongoing mechanical stress. Because bursitis can overlap with tendinitis, arthritis, joint infection, or muscle injury, getting the diagnosis right matters.
Table of Contents
- What Is Bursitis? Simple medical definition
- Bursitis at a glance
- Common bursitis types
- Bursitis symptoms (what it feels like)
- Causes & risk factors
- How bursitis is recognized
- Comorbidities & related conditions
- Prognosis (what to expect long-term)
- Understanding bursitis: complete condition explanation
- Bursitis vs tendinitis
- Diagnosis: exam, imaging, aspiration
- Treatment: symptom relief + cause-directed care
- Treatment targets (pain, swelling, function)
- Bursitis vs arthritis (quick table)
- When to seek urgent care
- Downloadable bursitis symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Bursitis? Simple Medical Definition
Bursitis is inflammation, swelling, or irritation of a bursa, a synovium-lined sac that cushions tissues and reduces friction around joints and bony prominences. In short, clinically, what is bursitis? It is a painful soft-tissue condition in which a bursa becomes swollen and tender, often due to overuse, pressure, trauma, crystal disease, inflammatory disease, or infection.
Bursitis at a Glance
Pain near a joint Pain often appears where tendons or soft tissues glide over bone
Swelling or tenderness The area may feel puffy, sore, or warm
Movement can hurt Activity, pressure, or certain positions often make symptoms worse
Overuse is common Repetitive movement or frequent pressure often triggers it
Infection is possible Some cases, especially around the elbow or knee, can become septic
Bursitis is often treatable and many cases improve with conservative care, but red, hot, or infected bursitis needs prompt evaluation.
Common Bursitis Types
Bursitis is usually named by the body area involved. Some types are strongly linked to repetitive movement, while others are more associated with kneeling, leaning on elbows, pressure from shoes, or inflammatory disease. Knowing the location helps guide the exam, possible causes, and best treatment approach.
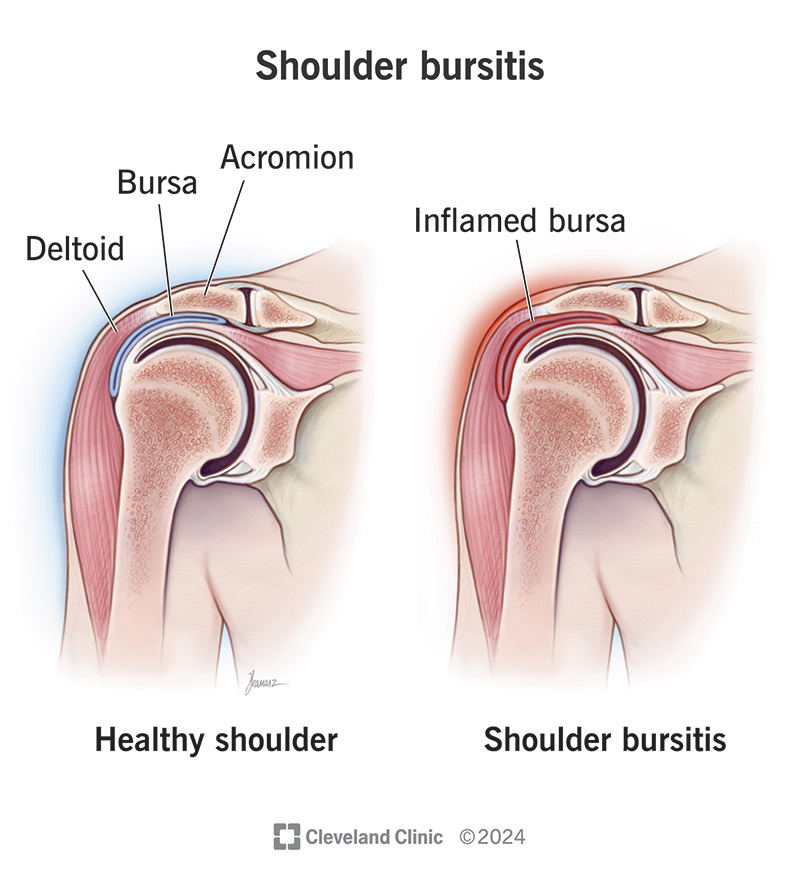
Shoulder bursitis Often causes pain lifting the arm or reaching overhead
Elbow bursitis Swelling over the tip of the elbow is common
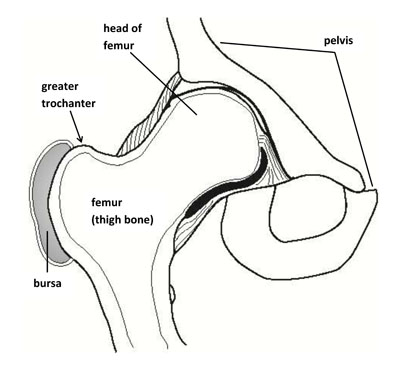
Hip bursitis Outer-hip pain may worsen with walking or lying on that side
Knee bursitis Front-of-knee swelling is common after kneeling or repeated pressure
Heel bursitis Pain near the Achilles tendon or back of the heel may occur
Bursitis symptoms (what it feels like)
Typical bursitis symptoms include pain, tenderness, swelling, warmth, and discomfort with movement or pressure on the affected area. Some patients notice a clearly swollen lump, especially at the elbow or knee, while others mainly feel aching, stiffness, or sharp pain with certain motions. Septic bursitis may also cause redness, increasing warmth, fever, or rapidly worsening swelling.
Shoulder • Elbow • Hip • Knee • Heel • Around major joints and bony pressure points
Overuse, pressure
Injury or infection
Fluid buildup
Inflammation
Pain, swelling
Tender movement
Find cause
Restore function
Wheel shows a simplified pathway: friction, pressure, injury, or infection → bursa irritation and swelling → pain and limited movement → cause-directed treatment.
Images for patient education
Shoulder bursitis
Elbow or knee swelling

Hip pain with movement
Causes & risk factors
Bursitis is commonly caused by repetitive motion, prolonged pressure, overuse, direct trauma, or friction around a joint. Some cases are linked to infection, gout, rheumatoid arthritis, other inflammatory diseases, or crystal deposition conditions. Risk often rises with certain jobs, sports, postures, kneeling, leaning on elbows, ill-fitting footwear, or movement patterns that repeatedly irritate the same area.
- Repetitive motion or overuse
- Direct pressure, kneeling, or leaning on joints
- Minor trauma or injury
- Infection in some superficial bursae
- Gout, pseudogout, or inflammatory arthritis
- Poor mechanics, tight tissues, or repetitive work demands
Evidence-based references (guidelines + high-quality sources)
General patient education: Mayo Clinic. Diagnosis and treatment: Mayo Clinic diagnosis and treatment. Clinical overview: Cleveland Clinic.
How Bursitis Is Recognized
Bursitis is usually recognized from the location of pain, the pattern of swelling or tenderness, and the way symptoms change with movement or pressure. Clinicians often diagnose it with a medical history and physical examination alone, especially when the presentation is classic. Additional testing may be needed when infection, arthritis, tendon injury, fracture, or another cause is possible.
Localized pain near a joint
Tenderness over a bursa
Swelling or fluid collection in some cases
Worse symptoms with pressure, motion, or overuse
Warmth or redness if inflammation is strong or infection is present
Imaging or aspiration when the diagnosis is unclear or infection is suspected
Comorbidities & related conditions
Bursitis may coexist with tendinitis, osteoarthritis, rheumatoid arthritis, gout, pseudogout, or movement-related soft tissue problems. In some patients, the bursa becomes irritated because nearby tendons are weak, a joint is stiff, or body mechanics put repeated strain on one spot. Identifying the related problem helps reduce recurrence rather than only treating the current flare.
- Tendinitis or rotator cuff disease
- Osteoarthritis or joint overload
- Gout or crystal-related inflammation
- Rheumatoid arthritis or other inflammatory disease
- Poor posture, weak stabilizing muscles, or repetitive strain
- Recurrent episodes if the trigger is not corrected
Prognosis (what to expect long-term)
Most cases of bursitis improve with conservative treatment over days to weeks, though some cases last longer depending on the location and ongoing trigger. Symptoms may return if repetitive stress, poor mechanics, or pressure on the area continues. Infected bursitis, recurrent bursitis, or bursitis linked to inflammatory disease usually needs closer follow-up and more targeted treatment.
Many cases settle with rest, ice, and reduced irritation.
Recovery may take longer if pressure, overuse, or inflammation continues.
Recurrent or infected bursitis needs more specific evaluation.
Understanding Bursitis: Complete Condition Explanation
A bursa acts like a small cushion that helps tissues glide smoothly over bone. When that bursa is irritated, it can swell, fill with extra fluid, and become painful with pressure or motion. This explains why bursitis often hurts most during movement, direct contact, or after the same motion is repeated over and over.
What happens in the bursa?
The bursa lining becomes irritated and may produce more fluid, which increases pressure in the small sac. As the surrounding tissues move, they rub against this swollen structure and trigger more pain. If bacteria enter the bursa, especially in a superficial location such as the elbow, the swelling can become septic bursitis and need urgent treatment.
Repeated friction, pressure, trauma, crystals, or infection → bursa irritation and fluid buildup → pain, swelling, and reduced joint comfort.
Bursitis vs tendinitis
Bursitis and tendinitis often occur near the same areas and can feel similar, but they affect different structures. Bursitis affects the fluid-filled sac that cushions movement, while tendinitis affects the tendon itself. Some patients actually have both at the same time, which is why careful exam and imaging can matter in persistent cases.
Bursa pain may be more pressure-related or linked to a focal swollen sac.
Tendon pain often follows resisted motion or tendon loading.
Correct diagnosis helps guide whether treatment should focus more on rest, injections, rehab, or tendon strengthening.
Diagnosis: exam, imaging, aspiration
Bursitis is usually diagnosed with a physical exam and medical history. X-rays do not show bursitis directly, but they may help rule out other problems, while ultrasound or MRI can identify swollen bursae when the diagnosis is unclear. If infection is suspected, clinicians may order blood tests or aspirate fluid from the bursa for analysis.
Tests often ordered during initial evaluation
Tests are chosen based on where the pain is located and whether infection or another disease is suspected.
- Physical examination to identify the tender bursa and assess range of motion.
- X-ray to rule out fracture, arthritis, bone spur, or another structural cause.
- Ultrasound or MRI when the diagnosis is uncertain or deeper bursae are involved.
- Blood tests if infection, gout, or inflammatory disease is suspected.
- Aspiration of bursal fluid when septic bursitis or crystal disease is a concern.
Treatment: symptom relief + cause-directed care
Effective bursitis treatment has two main goals: reduce pain and swelling, and correct the trigger that caused the bursa to become irritated. Many patients improve with conservative care such as rest, ice, activity modification, and over-the-counter pain relievers. Persistent, recurrent, infected, or mechanically complex cases may need aspiration, corticosteroid injection, physical therapy, antibiotics, or occasionally surgery.
1) Symptom control (short-term relief)
Resting the area, avoiding the triggering movement, applying ice, and using pain relievers such as NSAIDs or acetaminophen are common first steps. Padding, bracing, footwear changes, or avoiding direct pressure can also help depending on the location. These measures are often enough for simple overuse bursitis.
2) Long-term management (preventing recurrence)
Long-term management focuses on fixing the underlying reason the bursa keeps getting irritated. This may include stretching, strengthening, improving posture or biomechanics, physical therapy, work-activity adjustments, or treatment of gout, arthritis, or another inflammatory condition. Corticosteroid injections may help selected noninfectious cases, but they are not the right treatment when infection is present.
3) When additional treatment is needed
- Antibiotics are used when bursitis is infected.
- Aspiration can reduce pressure and help confirm infection or crystals.
- Physical therapy may improve range of motion and reduce recurring strain.
- Corticosteroid injection may be considered in selected noninfectious bursitis.
- Surgery is rare but may be considered when symptoms persist for months despite appropriate care.
Treatment targets (pain, swelling, function)
In bursitis, treatment targets focus on reducing local inflammation, improving movement, and preventing the problem from returning. Clinicians track pain level, tenderness, swelling, range of motion, activity tolerance, and whether signs of infection are present. Good control means the patient can move more comfortably, sleep better, return to daily activities, and avoid repeated flares.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Pain and irritation | Pain with movement, tenderness, pressure sensitivity, sleep disruption | Less pain and easier daily function |
| Swelling and inflammation | Warmth, fluid buildup, visible swelling, redness, infection clues | Reduced swelling and safer tissue status |
| Function and recurrence prevention | Range of motion, walking or lifting tolerance, work/sport triggers, biomechanics | Better movement and fewer repeat flares |
Case Study 1 (Example)
Patient developed outer-hip pain that worsened when lying on one side and walking longer distances. Evaluation suggested bursitis rather than hip arthritis or a fracture.hip- arthritis or a fracture.
Bursitis vs arthritis (quick comparison)
Bursitis and arthritis both cause joint-area pain, but they are not the same. Bursitis affects the soft tissue sac near a joint, while arthritis affects the joint itself. This distinction matters because swelling location, movement pattern, imaging, and treatment can be different.
| Feature | Bursitis | Arthritis |
|---|---|---|
| Main structure involved | Bursa near a joint | Joint surfaces and joint lining |
| Pain pattern | Often focal and worse with pressure or certain movement | Often more joint-centered with stiffness or grinding depending on type |
| Swelling | May be localized over a bursa | May involve the whole joint |
| Common causes | Overuse, pressure, trauma, infection, crystals | Wear-and-tear, inflammation, autoimmune disease, crystals |
| Treatment focus | Reduce local irritation and remove the trigger | Treat the joint disease causing inflammation or damage |
When to seek urgent care
- Fever, chills, major redness, or rapidly worsening swelling near the joint.
- Inability to move the joint normally or severe sudden pain.
- Drainage, broken skin, or concern for infection after trauma or pressure injury.
- Persistent symptoms that are not improving after 1 to 2 weeks of self-care or that keep returning.
Call Now for Bursitis Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “I thought I had simple joint pain, but the swelling and tenderness kept coming back. The team explained that it was bursitis and helped me fix the activities that were triggering it.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Bursitis is a common and often treatable cause of pain and swelling near a joint. If you have focal joint-area pain, swelling, tenderness, or symptoms that keep returning, a medical evaluation can help confirm the diagnosis, rule out infection, and start the right treatment plan.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always seek prompt care for fever, severe redness, drainage, or suspected infected bursitis.
© 2026 Rheumatology Care Associates. All rights reserved.