Medically reviewed by Dr. Priya Prakash (Rheumatologist, board certified) | Last updated: March 20, 2026
What Is Systemic Lupus Erythematosus (SLE)? Symptoms, Causes, Diagnosis & Treatment
Systemic lupus erythematosus (SLE) is a chronic autoimmune disease in which the immune system attacks healthy tissues in many parts of the body. Lupus can affect the skin, joints, kidneys, blood cells, lungs, heart, brain, and other organs, and symptoms can flare and settle over time. Early diagnosis and ongoing treatment can reduce flares, limit organ damage, and improve quality of life.
If you’re searching what is lupus or what is systemic lupus erythematosus, the simplest answer is that SLE is a multisystem autoimmune disease with a wide range of symptoms and severity levels. Some patients mainly have fatigue, rash, and joint pain, while others develop kidney inflammation, blood-count abnormalities, chest inflammation, neurologic symptoms, or other organ involvement. A rheumatologist can help confirm the diagnosis and create an individualized lupus treatment plan based on which organs are affected, how active the disease is, and the patient’s goals for safety and long-term control.
Lupus is often described as a disease of “many faces” because symptoms can vary greatly from one person to another and may change over time. It can cause flares and remissions, and not every patient has the same combination of skin, joint, kidney, or systemic features. Because SLE can mimic infections, thyroid disease, fibromyalgia, rheumatoid arthritis, vasculitis, or other autoimmune conditions, getting the diagnosis right matters.
Table of Contents
- What Is Systemic Lupus Erythematosus? Simple medical definition
- Lupus at a glance
- Common lupus patterns
- Lupus symptoms (what it feels like)
- Causes & risk factors
- How lupus is recognized
- Comorbidities & whole-body impact
- Prognosis (what to expect long-term)
- Understanding lupus: complete disease explanation
- Lupus vs rheumatoid arthritis
- Diagnosis: exam, labs, testing
- Treatment: symptom relief + long-term disease control
- Treatment targets (flare control, organ protection, remission)
- Lupus vs fibromyalgia (quick table)
- When to seek urgent care
- Downloadable lupus symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Systemic Lupus Erythematosus? Simple Medical Definition
Systemic lupus erythematosus (SLE) is a chronic systemic autoimmune disease characterized by immune dysregulation, autoantibody formation, and inflammation affecting multiple organs. In short, clinically, what is systemic lupus erythematosus? It is a relapsing-remitting autoimmune disease in which the immune system attacks the body’s own tissues, causing variable symptoms that can involve the skin, joints, kidneys, blood, lungs, heart, brain, and more.
Lupus at a Glance
Multisystem disease Skin, joints, kidneys, blood, lungs, and brain can be affected
Flares and remissions Symptoms may worsen and improve over time
Autoimmune activity The immune system attacks healthy tissues
Common early symptoms Fatigue, rash, joint pain, fevers, and mouth ulcers may appear first
Needs long-term monitoring Organ involvement can develop even when symptoms seem mild
Lupus is not one single symptom pattern. It is a variable autoimmune disease that may range from mild skin-joint disease to serious organ-threatening illness.
Common Lupus Patterns
SLE can present in many different ways, which is one reason diagnosis can be challenging. Some patients have mainly skin and joint disease, while others develop kidney inflammation, blood abnormalities, serositis, neurologic involvement, or antiphospholipid-related problems. Clinicians often think about lupus by the main organ systems involved, disease activity level, and whether the current problem reflects an acute flare, chronic damage, or medication complication.
Mucocutaneous lupus Rash, photosensitivity, hair loss, and mouth ulcers dominate
Musculoskeletal lupus Joint pain, swelling, and stiffness are prominent
Lupus nephritis Kidney inflammation causes protein loss, swelling, or abnormal urine findings
Systemic inflammatory lupus Blood, lungs, heart, or brain involvement becomes important
Relapsing-remitting lupus Symptoms flare and then partially settle over time
Lupus symptoms (what it feels like)
Typical lupus symptoms include fatigue, joint pain, rash, fever, and sensitivity to sunlight. Many patients notice joint aches or swelling, mouth ulcers, hair loss, chest pain with deep breathing, swollen glands, or fingers that change color in the cold. Some people also develop swelling of the legs, foamy urine, headaches, seizures, confusion, shortness of breath, anemia, low platelets, or other symptoms depending on which organs are involved.
Skin • Joints • Kidneys • Blood • Lungs • Heart • Brain • Mouth • Hair • Blood vessels
Genes, hormones
Environment
Autoantibodies
Immune complexes
Flares, rash
Pain, organ signs
Confirm SLE
Protect organs
Wheel shows a simplified pathway: immune dysregulation → autoantibody and immune-complex injury → lupus flare symptoms and organ involvement → evaluation and long-term control.
Images for patient education
Skin and rash symptoms
Joint and fatigue symptoms
Organ involvement
Causes & risk factors
Lupus develops because of a combination of genetic susceptibility, immune-system abnormalities, hormones, and environmental triggers. Ultraviolet light, infections, smoking, and certain medications can contribute in some patients, and the disease is much more common in women, especially during the childbearing years. The underlying immune process leads to autoantibody production and immune-complex deposition, which can damage tissues in many organ systems.
- Genetic predisposition and autoimmune susceptibility
- Female sex and hormonal influence patterns
- Sunlight or ultraviolet exposure as a common trigger
- Smoking or other environmental contributors
- Autoantibodies such as ANA, anti-dsDNA, anti-Smith, or antiphospholipid antibodies
- Immune-complex driven inflammation affecting multiple organs
Evidence-based references (guidelines + high-quality sources)
General patient education: RheumInfo. Clinical overview: NIAMS. Diagnosis and treatment overview: Mayo Clinic.
How Lupus Is Recognized
Lupus is recognized by the combination of symptoms, physical findings, autoimmune blood tests, and evidence of inflammation or organ involvement. Specialists often look for a pattern that may include rash, photosensitivity, mouth ulcers, joint inflammation, blood-count changes, kidney abnormalities, chest-lining inflammation, neurologic symptoms, and a positive ANA. The diagnosis can be difficult because symptoms often appear gradually, fluctuate over time, and overlap with many other conditions.
Photosensitive rash or skin disease
Joint pain, swelling, or morning stiffness
Mouth ulcers and hair loss
Blood-count abnormalities or inflammatory lab patterns
Kidney, lung, or nervous-system involvement in some patients
Positive ANA with more specific antibody support when present
Comorbidities & whole-body impact
Lupus can affect almost every part of daily life because it is a systemic inflammatory disease. Fatigue, pain, photosensitivity, kidney disease, cardiovascular risk, infections, blood clots, bone loss, mood burden, and medication side effects can all shape long-term outcomes. High-quality lupus care requires attention not only to flare control, but also to organ protection, pregnancy planning, vaccination safety, and treatment monitoring.
- Fatigue and reduced quality of life
- Lupus nephritis and kidney-damage risk
- Blood-count abnormalities and clotting risk
- Cardiovascular disease and bone-loss risk over time
- Infection risk from disease activity or immune-suppressing treatment
- Pregnancy-related planning needs in selected patients
Prognosis (what to expect long-term)
The outlook for lupus has improved greatly because of earlier diagnosis, better medications, and closer monitoring. Even so, the long-term course depends on which organs are involved, how severe flares are, how early treatment begins, and how well disease activity is controlled. The central goals are to prevent flares, limit permanent organ damage, reduce treatment toxicity, and support long-term quality of life.
Many patients live long lives with lupus when it is monitored carefully.
Serious kidney, brain, blood, or clotting involvement needs closer follow-up.
Good control means fewer flares, less damage, and safer long-term health.
Understanding Lupus: Complete Disease Explanation
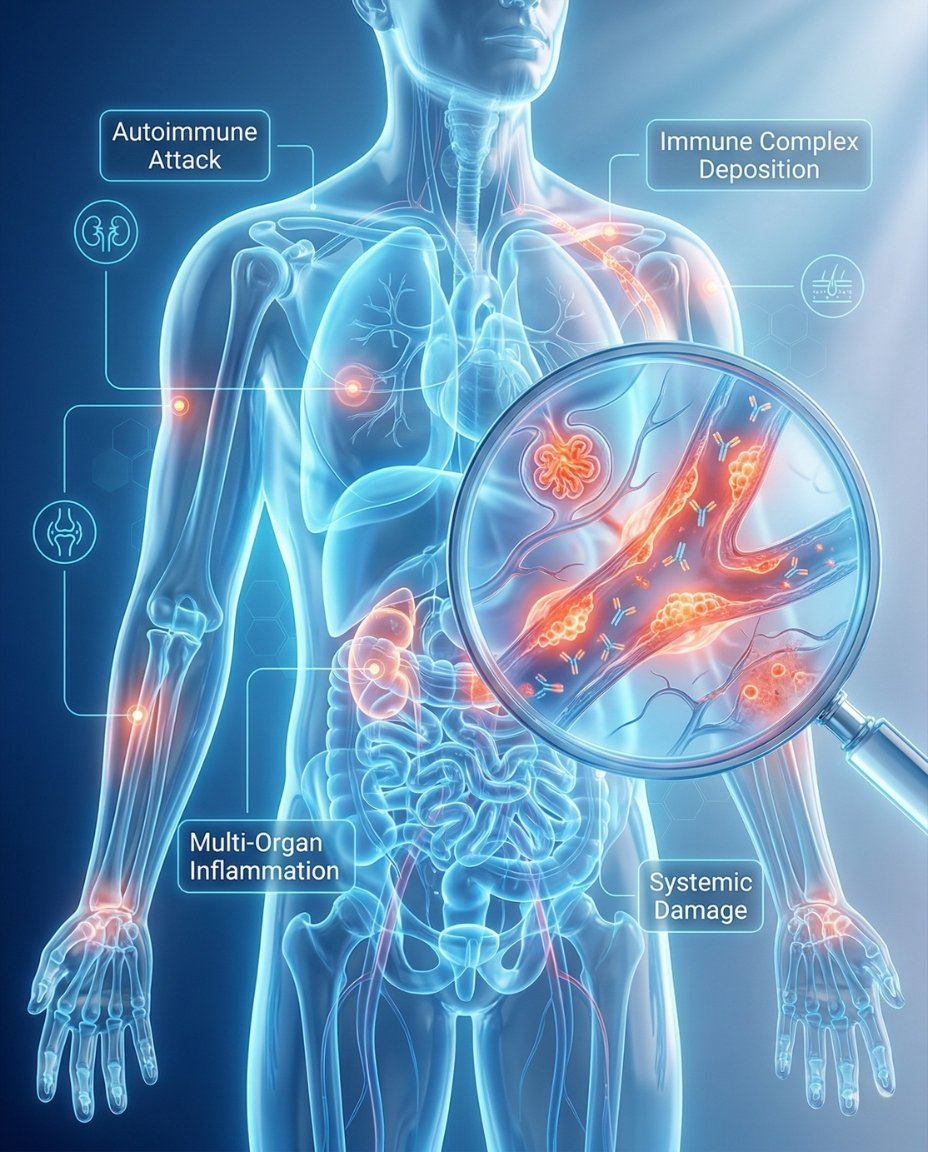
Lupus occurs when the immune system becomes abnormally activated and produces autoantibodies that target the body’s own tissues. These immune abnormalities can form immune complexes that deposit in organs and trigger inflammation. This helps explain why lupus can affect the skin, joints, kidneys, lungs, heart, blood, and nervous system rather than one single body part.
What happens at the immune and organ level?
In SLE, the immune system loses tolerance to self-antigens and produces a range of autoantibodies. These antibodies and the inflammatory pathways they activate can damage tissues directly or through immune-complex deposition. The final result is a disease that may flare unpredictably and show very different organ patterns from one patient to another.
Immune dysregulation → autoantibody formation → immune-complex inflammation → skin, joint, kidney, blood, lung, or brain involvement.
Lupus vs rheumatoid arthritis
Lupus and rheumatoid arthritis can both cause inflammatory joint pain, but they are not the same disease. Lupus is a multisystem autoimmune disease with wider organ involvement patterns, while RA more strongly centers on chronic erosive synovitis and joint damage. Distinguishing between them is important because the organ risks, blood-test profile, and treatment priorities can differ significantly.
Lupus often includes rash, photosensitivity, ulcers, blood-count changes, and kidney risk.
RA more classically causes symmetric inflammatory small-joint disease with erosive damage risk.
Correct classification helps guide organ monitoring and medication strategy.
Diagnosis: exam, labs, testing
Lupus is diagnosed using the overall clinical pattern, autoimmune blood tests, urine testing, and targeted organ evaluation. Doctors often order ANA first, then more specific tests such as anti-double-stranded DNA, anti-Smith, antiphospholipid antibodies, CBC, complement levels, urine protein testing, kidney-function tests, and inflammatory markers depending on the presentation. Because lupus can affect many organs, diagnosis and monitoring also depend on imaging, biopsy, or specialist testing when kidney, lung, heart, skin, or nervous-system disease is suspected.
Tests often ordered during initial evaluation
Tests help confirm the diagnosis, define which organs are involved, and guide treatment safety.
- Blood tests such as ANA, anti-dsDNA, anti-Smith, antiphospholipid antibodies, complement levels, CBC, ESR, and CRP.
- Urinalysis, urine protein measurement, and kidney-function blood tests to screen for lupus nephritis.
- Physical examination focused on rash, ulcers, swollen joints, edema, blood pressure, and neurologic signs.
- Imaging or specialist testing when chest pain, shortness of breath, seizures, or organ-specific symptoms are present.
- Kidney, skin, or other tissue biopsy in selected cases when organ-level confirmation is needed.
Treatment: symptom relief + long-term disease control
Effective lupus treatment has two main goals: control active inflammation and prevent irreversible organ damage. Treatment is tailored to the organs involved, which means mild skin-joint disease is managed differently from lupus nephritis, blood disorders, or central nervous system lupus. Hydroxychloroquine is a core medication for many patients, while corticosteroids, immunosuppressive drugs, and biologic therapies may be used depending on severity.
1) Symptom control (short-term relief)
Mild symptoms such as fever, aches, rash, or joint pain may be treated with supportive measures, NSAIDs in selected patients, and short-term corticosteroids when needed. Sun protection is also a critical part of symptom control because ultraviolet exposure commonly worsens lupus activity. Early symptom relief is helpful, but it should be paired with a long-term plan that reduces flare risk and protects organs.
2) Long-term management (disease control and organ protection)
Long-term treatment may include hydroxychloroquine, corticosteroid-sparing immunosuppressive medicines, biologics, anticoagulation in selected antiphospholipid cases, and organ-specific care depending on disease manifestations. The main goal is to keep disease activity as low as possible while minimizing medication toxicity and preventing flares. Long-term care also includes regular laboratory monitoring, urine checks, vaccination planning, sun protection, and pregnancy counseling when relevant.
3) Lifestyle strategies that support treatment
- Use daily sun protection and avoid excess ultraviolet exposure.
- Keep follow-up visits and laboratory testing because lupus can change even when symptoms seem quiet.
- Report swelling, chest pain, dark or foamy urine, severe headaches, or new neurologic symptoms promptly.
- Protect bone and cardiovascular health during long-term treatment, especially if corticosteroids are used.
- Discuss pregnancy planning early because lupus activity and medications need careful management.
Treatment targets (flare control, organ protection, remission)
In lupus, treatment targets focus on reducing flares, protecting organs, and keeping disease activity as low as safely possible. Clinicians track symptoms, exam findings, urine and blood tests, medication side effects, and organ-specific markers depending on whether the disease affects the kidneys, blood, skin, brain, lungs, or joints. Good control means fewer flares and better daily function, but it also means limiting cumulative organ damage over years.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Flare activity | Fatigue, rash, ulcers, joint symptoms, fever, serositis, symptom changes | Fewer and milder lupus flares |
| Immune and lab control | ANA context, anti-dsDNA, complement, CBC, ESR, CRP, urine findings | Stable or improving inflammatory and organ markers |
| Organ protection | Kidneys, blood pressure, lungs, heart, brain, clotting risk, medication safety | Preserved organ function and reduced long-term damage |
Case Study 1 (Example)
Patient developed joint pain, fatigue, and a butterfly-shaped rash across the cheeks and nose. Evaluation suggested lupus rather than skin- allergy or simple viral illness.
Lupus vs fibromyalgia (quick comparison)
Lupus and fibromyalgia can both cause fatigue and body pain, but they are very different conditions. Lupus is an autoimmune inflammatory disease that can damage organs, while fibromyalgia is a pain-processing disorder that does not cause the same immune-mediated organ inflammation. Distinguishing between them is especially important when a patient has fatigue and pain but only one condition is causing active inflammatory damage.
| Feature | Lupus | Fibromyalgia |
|---|---|---|
| Main mechanism | Autoimmune inflammation and autoantibodies | Central pain processing and sensitivity changes |
| Inflammation | Can affect skin, joints, kidneys, blood, lungs, brain | Does not cause organ inflammation |
| Blood or urine abnormalities | Often possible depending on disease activity | Not typical of fibromyalgia itself |
| Rash or photosensitivity | May occur | Not a defining feature |
| Treatment focus | Immune control and organ protection | Pain, sleep, exercise, and nervous-system symptom management |
When to seek urgent care
- Chest pain, shortness of breath, coughing blood, or severe pleuritic pain.
- Foamy urine, sudden swelling, reduced urination, or suspected kidney flare.
- Severe headache, confusion, seizure, weakness, or other neurologic symptoms.
- Blood-clot symptoms, severe infection symptoms, or rapidly worsening overall condition.
Call Now for Lupus Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “I had rashes, fatigue, joint pain, and abnormal labs but no one connected them at first. The team helped me understand lupus and start a real long-term plan.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Systemic lupus erythematosus is a complex but treatable autoimmune disease that can affect many organs and cause flares over time. If you have unexplained fatigue, rash, joint pain, mouth ulcers, photosensitivity, or kidney-related symptoms, a rheumatology evaluation can help confirm the diagnosis and build the right long-term treatment plan.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always seek prompt care for chest pain, kidney symptoms, neurologic symptoms, or signs of severe flare.
© 2026 Rheumatology Care Associates. All rights reserved.