Medically reviewed by Dr. Priya Prakash (Rheumatologist, board certified) | Last updated: March 20, 2026
What Is Rheumatoid Arthritis (RA)? Symptoms, Causes, Diagnosis & Treatment
Rheumatoid arthritis (RA) is a chronic autoimmune inflammatory disease that causes pain, swelling, stiffness, and joint damage. It most often affects the small joints of the hands, wrists, and feet in a symmetric pattern, but it can also affect other joints and organs. Early diagnosis and aggressive treatment can reduce inflammation, prevent damage, and improve the chance of remission.
If you’re searching what is rheumatoid arthritis, the simplest answer is that RA is an autoimmune disease in which the immune system attacks the lining of the joints. This causes chronic inflammation that can lead to pain, swelling, prolonged morning stiffness, and progressive joint damage if not treated. A rheumatologist can confirm the diagnosis and create an individualized rheumatoid arthritis treatment plan based on symptoms, blood tests, imaging, disease activity, and overall health.
arthritis
Rheumatoid arthritis commonly begins in the hands, wrists, and feet, often affecting the same joints on both sides of the body. It can also cause fatigue, low appetite, anemia, nodules, and inflammation affecting the lungs, eyes, blood vessels, or other body systems. Because RA can resemble osteoarthritis, psoriatic arthritis, lupus, viral arthritis, or other inflammatory joint diseases, getting the diagnosis right matters.
Table of Contents
- What Is Rheumatoid Arthritis? Simple medical definition
- Rheumatoid arthritis at a glance
- Common rheumatoid arthritis patterns
- Rheumatoid arthritis symptoms (what it feels like)
- Causes & risk factors
- How rheumatoid arthritis is recognized
- Comorbidities & whole-body impact
- Prognosis (what to expect long-term)
- Understanding rheumatoid arthritis: complete disease explanation
- RA vs osteoarthritis
- Diagnosis: exam, labs, imaging
- Treatment: symptom relief + long-term disease control
- Treatment targets (remission, inflammation, function)
- Rheumatoid arthritis vs lupus arthritis (quick table)
- When to seek urgent care
- Downloadable rheumatoid arthritis symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Rheumatoid Arthritis? Simple Medical Definition
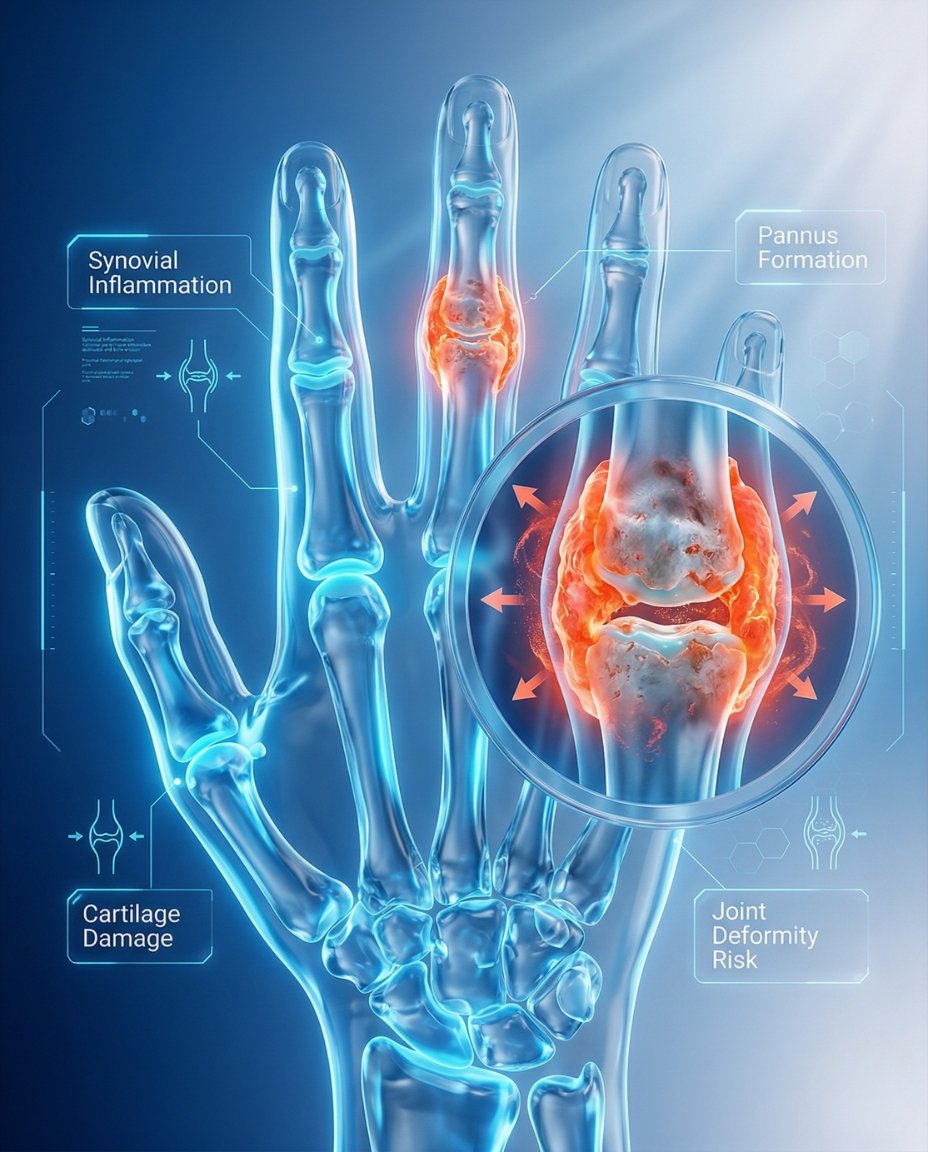
Rheumatoid arthritis (RA) is a chronic systemic autoimmune inflammatory arthritis that primarily targets the synovial lining of the joints. In short, clinically, what is rheumatoid arthritis? It is an immune-mediated disease that causes persistent synovitis, joint swelling, prolonged morning stiffness, progressive structural damage, and in some patients inflammation outside the joints as well.
Rheumatoid Arthritis at a Glance
Symmetric joint pattern Often affects the same joints on both sides of the body
Small joints common Hands, wrists, and feet are frequent early sites
Long morning stiffness Stiffness often lasts much longer than in osteoarthritis
Autoimmune inflammation Joint lining inflammation drives pain and damage
Whole-body disease Fatigue and extra-joint symptoms can also occur
RA is not only a joint pain condition. It is a systemic inflammatory disease that can affect daily function and long-term health if untreated.
Common Rheumatoid Arthritis Patterns
Rheumatoid arthritis can vary in how it starts, which joints it affects first, and how aggressive the disease becomes over time. Some patients develop classic symmetric small-joint disease, while others begin with a more limited pattern that later spreads. Clinicians often think about RA by serostatus, severity, disease activity, early versus established disease, and whether there are extra-articular features.
Early RA New inflammatory joint symptoms with limited structural damage
Established RA Persistent disease with clearer swelling, stiffness, and imaging change
Seropositive RA RF or anti-CCP antibodies are present
Seronegative RA Typical inflammatory arthritis pattern without positive antibodies
Extra-articular RA Lungs, eyes, nodules, blood vessels, or other systems are involved
Rheumatoid arthritis symptoms (what it feels like)
Typical rheumatoid arthritis symptoms include joint pain, swelling, warmth, and prolonged morning stiffness. Many patients notice stiffness that lasts more than 30 to 60 minutes, trouble making a fist, reduced grip strength, or painful swelling in the wrists, knuckles, fingers, or forefeet. Some people also develop fatigue, low-grade fever, reduced appetite, anemia, rheumatoid nodules, and other systemic symptoms as inflammation continues.
Hands • Wrists • Fingers • Feet • Toes • Knees • Ankles • Elbows • Shoulders
Genes, smoking
Immune triggers
Synovial inflammation
Persistent immune attack
Swelling, stiffness
Fatigue, pain
Confirm RA
Treat-to-target plan
Wheel shows a simplified pathway: autoimmune synovial inflammation → painful swollen stiff joints → evaluation and long-term disease control.
Images for patient education
Hand joint swelling
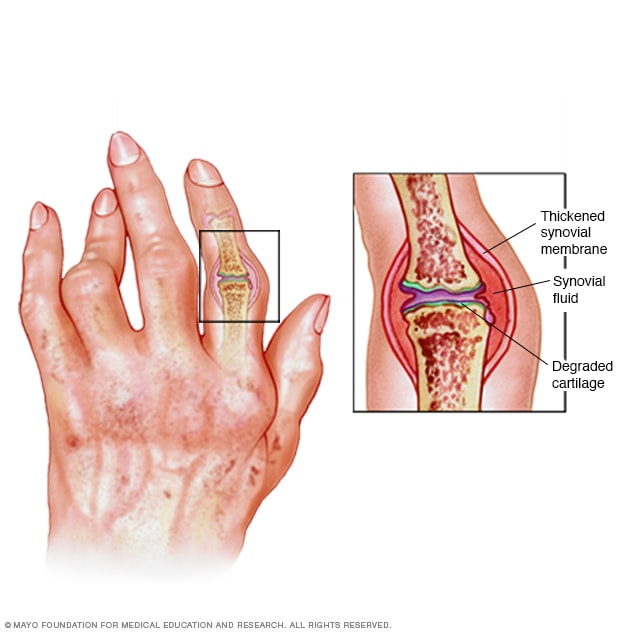
Synovial inflammation
Morning stiffness

Causes & risk factors
RA is an autoimmune disease, which means the immune system mistakenly attacks healthy joint tissue. The exact cause is not fully known, but genetics, smoking, hormonal factors, and environmental exposures all appear to contribute to disease risk. Over time, the immune attack causes chronic synovial inflammation that can damage cartilage, bone, tendons, and joint structure.
- Family or genetic predisposition in some patients
- Smoking, a major modifiable risk factor
- Autoimmune activation against joint tissues
- Positive RF or anti-CCP antibodies in many patients
- Systemic inflammation that can affect organs outside the joints
- Need for early treatment to reduce irreversible damage risk
Evidence-based references (guidelines + high-quality sources)
General patient education: RheumInfo. Clinical overview: NIAMS. Diagnosis and treatment review: Mayo Clinic.
How Rheumatoid Arthritis Is Recognized
Rheumatoid arthritis is recognized by the pattern of inflammatory joint symptoms, physical exam findings, blood tests, and imaging support. Specialists often look for joint swelling, prolonged morning stiffness, symmetric involvement, tenderness of the small joints, and symptoms lasting more than a brief flare. RA can be difficult to diagnose early because there is no single test that proves every case, especially in the first months of disease.
Symmetric small-joint pain and swelling
Prolonged morning stiffness
Warm tender joints on exam
Positive anti-CCP or RF in many patients
Ultrasound, MRI, or X-ray support when needed
Persistent inflammatory pattern rather than mechanical pain alone
Comorbidities & whole-body impact
RA is a systemic disease, not only a joint disease. It can affect fatigue level, work ability, sleep, mood, cardiovascular risk, bone health, lung function, and quality of life, and some patients develop extra-articular disease in organs outside the joints. High-quality RA care includes attention to inflammation control, physical function, medication safety, and broader health risks that accompany chronic autoimmune disease.
- Fatigue and reduced endurance
- Functional limitation in work, self-care, and hand use
- Rheumatoid nodules in some patients
- Lung, eye, blood-vessel, or other extra-articular involvement
- Increased cardiovascular and osteoporosis risk over time
- Treatment side effects that require regular monitoring
Prognosis (what to expect long-term)
The long-term outlook for RA has improved substantially because of earlier diagnosis and better treatment strategies. Even so, untreated or undertreated disease can lead to permanent joint damage, deformity, disability, and broader systemic complications. The goal is to treat early, control inflammation tightly, and aim for remission or very low disease activity as soon as safely possible.
Early treatment can greatly improve long-term outcomes.
Many patients can reach low disease activity or remission with modern therapy.
Ongoing monitoring remains important because disease activity and medication needs can change over time.
Understanding Rheumatoid Arthritis: Complete Disease Explanation
Rheumatoid arthritis begins when the immune system targets the synovium, the tissue lining the joints. The inflamed synovium thickens and can gradually damage cartilage, bone, tendons, and ligaments if inflammation is not controlled. This process explains why RA causes joint pain and swelling at first, but can later lead to deformity and loss of function if treatment is delayed.
What happens inside the joint?
In RA, persistent immune activation drives chronic synovitis. The inflamed synovial tissue can invade nearby cartilage and bone, leading to erosions and structural damage over time. This is why early anti-inflammatory disease control is so important, even when symptoms still seem “mild.”
Autoimmune synovial attack → chronic joint inflammation → cartilage and bone damage → pain, stiffness, swelling, and long-term functional loss if uncontrolled.
RA vs osteoarthritis
RA and osteoarthritis both affect joints, but they are very different diseases. RA is an autoimmune inflammatory arthritis, while osteoarthritis is primarily a degenerative whole-joint disorder related to tissue wear, joint mechanics, and aging-related change. The difference matters because RA needs early immune-targeting treatment, while osteoarthritis is managed with a very different long-term strategy.
RA usually causes prolonged morning stiffness, swelling, and inflammatory symptoms.
OA more often causes mechanical pain that worsens with use and has shorter stiffness after rest.
Correct diagnosis helps guide early DMARD therapy when RA is present.
Diagnosis: exam, labs, imaging
Rheumatoid arthritis is diagnosed using the overall pattern of symptoms, physical examination, laboratory testing, and imaging. Doctors commonly evaluate joint swelling and tenderness, symptom duration, inflammatory markers, rheumatoid factor, anti-CCP antibodies, and imaging such as X-rays, ultrasound, or MRI. Imaging can be especially helpful when symptoms are early or when clinicians need to look for synovitis or erosive change not yet obvious on standard exam.
Tests often ordered during initial evaluation
Tests help support the diagnosis, assess severity, and guide treatment safety.
- Blood tests such as ESR, CRP, rheumatoid factor, and anti-CCP antibodies.
- Complete blood count and chemistry testing to assess anemia, inflammation, and treatment safety baseline.
- X-rays, ultrasound, or MRI to evaluate synovitis, erosions, and structural change.
- Physical exam of swollen and tender joint count, hand function, and range of motion.
Treatment: symptom relief + long-term disease control
Effective rheumatoid arthritis treatment has two main goals: relieve current symptoms and stop inflammation from causing joint damage. Modern RA care uses a treat-to-target strategy, which means treatment is adjusted until the patient reaches remission or very low disease activity whenever possible. DMARD therapy is the foundation of long-term control, while short-term relief may also include NSAIDs, corticosteroids, or other supportive measures depending on the situation.
1) Symptom control (short-term relief)
NSAIDs or short courses of corticosteroids may help reduce pain and inflammation while longer-term medicines begin working. These short-term tools can improve daily function, but they do not replace disease-modifying treatment. The goal is to bridge symptoms safely while building a long-term plan that actually suppresses the disease process.
2) Long-term management (disease modification)
DMARDs such as methotrexate are central to RA treatment, and some patients also need combination DMARD therapy, biologics, or targeted synthetic drugs depending on disease severity and response. Treatment is usually adjusted based on disease activity, imaging progression, side effects, and the patient’s goals for function and quality of life. Regular follow-up is essential because the best outcomes come from tight monitoring and timely adjustment, not from a one-time prescription alone.
3) Lifestyle strategies that support treatment
- Stop smoking, because smoking increases RA risk and can reduce treatment success.
- Use regular movement, hand exercise, and physical therapy when stiffness or weakness reduces function.
- Protect cardiovascular and bone health as part of long-term RA care.
- Keep all follow-up and laboratory monitoring appointments when taking DMARDs or biologic medication.
- Report persistent fever, infection concerns, breathing symptoms, or major medication side effects promptly.
Treatment targets (remission, inflammation, function)
In RA, treatment targets focus on achieving remission or at least very low disease activity. Clinicians track swollen joints, tender joints, patient symptoms, inflammatory markers, function, and imaging progression to see whether treatment is working well enough. Good control means less pain and stiffness, but it also means preventing future structural damage and preserving long-term function.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Inflammation symptoms | Joint swelling, tenderness, morning stiffness, fatigue | Minimal active synovitis and easier daily movement |
| Disease activity | Clinical scores, ESR/CRP, flare pattern, medication response | Remission or very low disease activity |
| Long-term protection | Imaging progression, hand function, organ involvement, treatment safety | Stable joints, preserved function, and limited long-term damage |
Case Study 1 (Example)
Patient developed symmetrical joint pain and swelling in the hands with prolonged morning stiffness. Evaluation suggested rheumatoid arthritis rather than age-related- joint pain or osteoarthritis.
Rheumatoid arthritis vs lupus arthritis (quick comparison)
RA and lupus can both cause inflammatory joint pain, but they are not the same disease. RA more strongly targets the joints with persistent synovitis and damage risk, while lupus arthritis is often part of a broader systemic autoimmune illness with different organ patterns and treatment priorities. Distinguishing between them helps guide testing, monitoring, and long-term therapy choices.
| Feature | Rheumatoid arthritis (RA) | Lupus arthritis |
|---|---|---|
| Main pattern | Chronic inflammatory synovitis with damage risk | Inflammatory joint symptoms as part of systemic lupus |
| Joint damage | Can be erosive and destructive if untreated | Often less erosive, though still clinically important |
| Typical blood tests | RF and anti-CCP may be positive | ANA and lupus-specific antibodies are often relevant |
| Extra-joint pattern | Lungs, nodules, eyes, vascular complications may occur | Skin, kidneys, blood counts, serositis, CNS and more may be involved |
| Treatment approach | DMARD-based treat-to-target arthritis control | Lupus-directed immune management based on organ involvement |
When to seek urgent care
- Rapidly worsening swelling and severe pain with fever, because joint infection must be ruled out.
- Shortness of breath, chest pain, or serious systemic symptoms that may reflect extra-articular disease or treatment complications.
- New neurologic symptoms, severe eye symptoms, or marked weakness.
- Signs of serious infection while taking immunosuppressive treatment.
Call Now for Rheumatoid Arthritis Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My hands were swollen and stiff every morning and I thought it would just pass. The team diagnosed my RA early and helped me start treatment before things got worse.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
FAQ
Conclusion
Rheumatoid arthritis is a treatable autoimmune inflammatory disease, but it can cause permanent joint damage and systemic complications if therapy is delayed. If you have persistent swollen stiff joints, especially in a symmetric pattern involving the hands, wrists, or feet, an early rheumatology evaluation can help confirm the diagnosis and start the right long-term treatment plan.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always seek prompt care for severe swelling with fever, breathing symptoms, or suspected medication-related infection.
© 2026 Rheumatology Care Associates. All rights reserved.