Medically reviewed by Dr. Priya Prakash (Rheumatologist, board certified) | Last updated: March 20, 2026
What Is Osteoarthritis (OA)? Symptoms, Causes, Diagnosis & Treatment
Osteoarthritis (OA) is the most common type of arthritis and happens when the tissues inside a joint gradually break down over time. It most often affects the knees, hips, hands, and spine, and it can cause pain, stiffness, swelling, reduced movement, and loss of function. Early recognition and a structured treatment plan can reduce pain, improve mobility, and help protect long-term joint function.
If you’re searching what is osteoarthritis, the simplest answer is that OA is a long-term joint condition in which cartilage and other joint structures wear down over time. As the joint changes, movement can become painful, stiff, or less flexible, especially after activity or after periods of rest. A rheumatologist or other musculoskeletal specialist can help confirm the diagnosis and create an individualized osteoarthritis treatment plan based on the joints involved, symptom severity, and impact on daily life.
Arthritis
Many people notice gradually increasing joint pain, morning stiffness that improves within a short time, and discomfort that gets worse after use. OA can also lead to creaking, tenderness, reduced range of motion, trouble walking, weaker surrounding muscles, and sleep disruption when pain becomes persistent. Because joint pain can also come from inflammatory arthritis, bursitis, tendon disorders, or referred pain, getting the diagnosis right matters.
Table of Contents
- What Is Osteoarthritis? Simple medical definition
- Osteoarthritis at a glance
- Common osteoarthritis patterns
- Osteoarthritis symptoms (what it feels like)
- Causes & risk factors
- How osteoarthritis is recognized
- Comorbidities & whole-body impact
- Prognosis (what to expect long-term)
- Understanding osteoarthritis: complete disease explanation
- OA vs inflammatory arthritis
- Diagnosis: exam, labs, imaging
- Treatment: symptom relief + long-term joint care
- Treatment targets (pain, movement, function)
- Osteoarthritis vs rheumatoid arthritis (quick table)
- When to seek urgent care
- Downloadable osteoarthritis symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Osteoarthritis? Simple Medical Definition
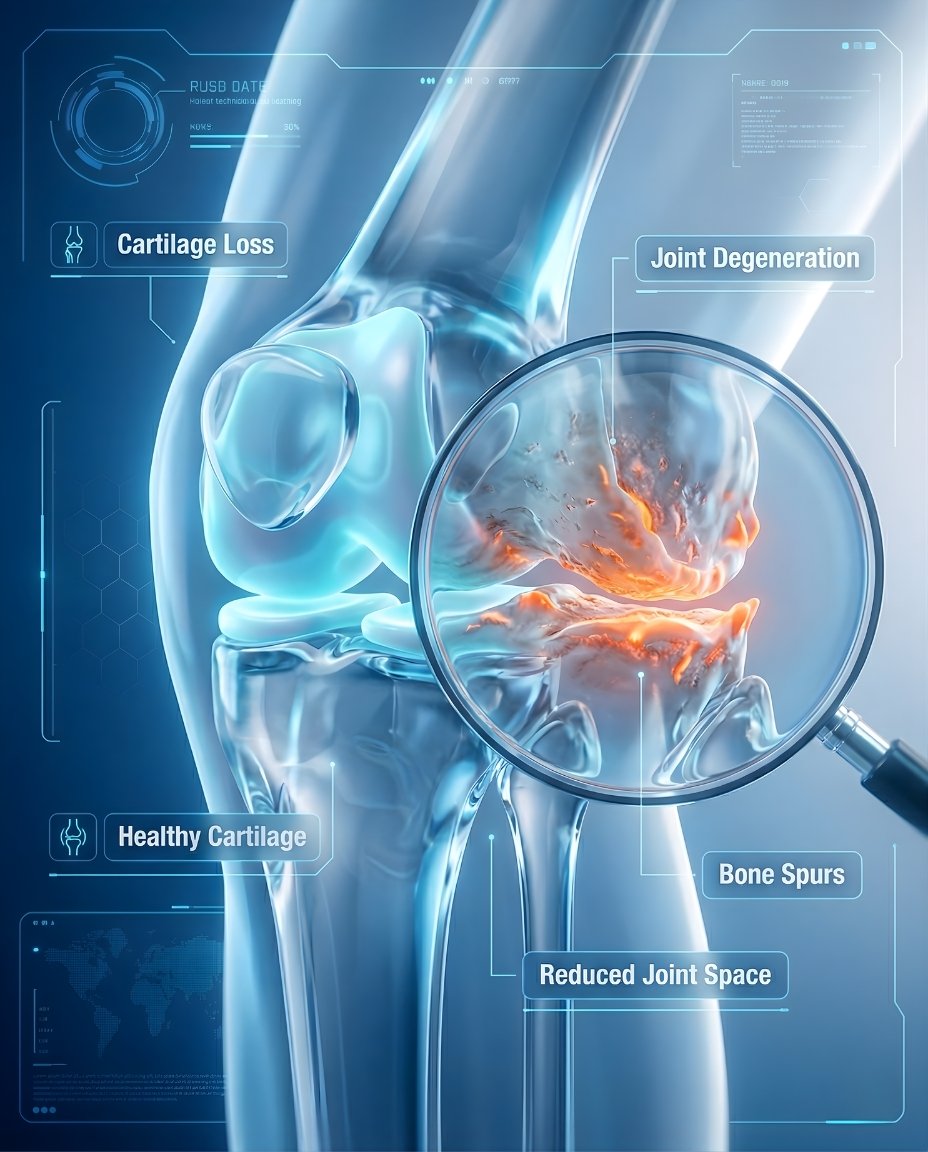
Osteoarthritis (OA) is a chronic degenerative joint disease in which cartilage and other tissues within the joint gradually break down over time. In short, clinically, what is osteoarthritis? It is a whole-joint disorder involving cartilage loss, bony change, joint lining irritation, and altered joint mechanics that can cause pain, stiffness, swelling, and reduced function.
Osteoarthritis at a Glance
Pain with use Symptoms often worsen with activity or after overuse
Short morning stiffness Stiffness usually lasts less than 30 minutes
Common joints Knees, hips, hands, and spine are frequently affected
Reduced movement Joints may feel tight, weak, or less flexible
Gradual progression Symptoms usually build slowly over time
OA is often described as “wear-and-tear” arthritis, but it actually affects the entire joint, not only cartilage.
Common Osteoarthritis Patterns
Osteoarthritis can look different depending on which joint is involved and how much the disease affects movement, strength, and daily tasks. Clinicians often think about OA by location, severity, and whether symptoms are mostly mechanical, function-limiting, or advanced enough to affect sleep and routine mobility.
Knee OA Pain with stairs, walking, squatting, or standing up
Hip OA Groin pain, stiffness, limping, trouble putting on shoes
Hand OA Finger pain, bony nodes, grip weakness, hand stiffness
Spine OA Neck or low back pain with stiffness and reduced motion
Multi-joint OA More than one region affected over time
Osteoarthritis symptoms (what it feels like)
Typical osteoarthritis symptoms include joint pain, stiffness after rest, tenderness, reduced flexibility, and discomfort that tends to worsen with joint use. Morning stiffness is usually brief compared with inflammatory arthritis, and many patients describe a “getting going” stiffness after sitting for a while. As OA becomes more advanced, some people also notice swelling, creaking or grinding, joint enlargement, weakness around the joint, and pain that starts to interfere with sleep or day-to-day function.
Knees • Hips • Hands • Fingers • Neck • Low back • Feet • Big toe base
Age, weight
Joint stress
Cartilage loss
Bone remodeling
Pain, stiffness
Less mobility
Confirm OA
Treatment plan
Wheel shows a simplified pathway: joint stress and tissue breakdown → pain and stiffness → evaluation and long-term management.
Images for patient education
Knee OA pain
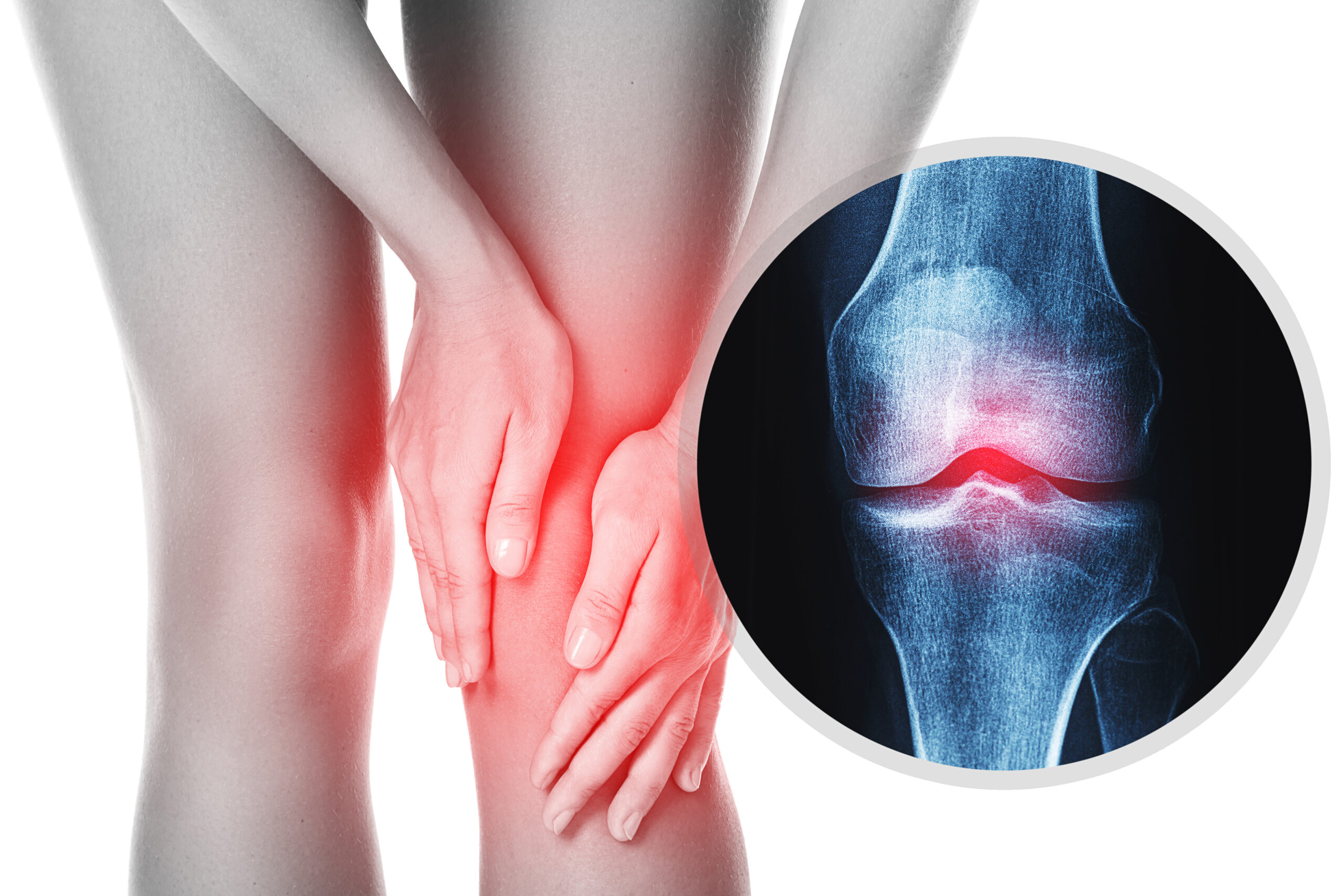
Joint wear changes
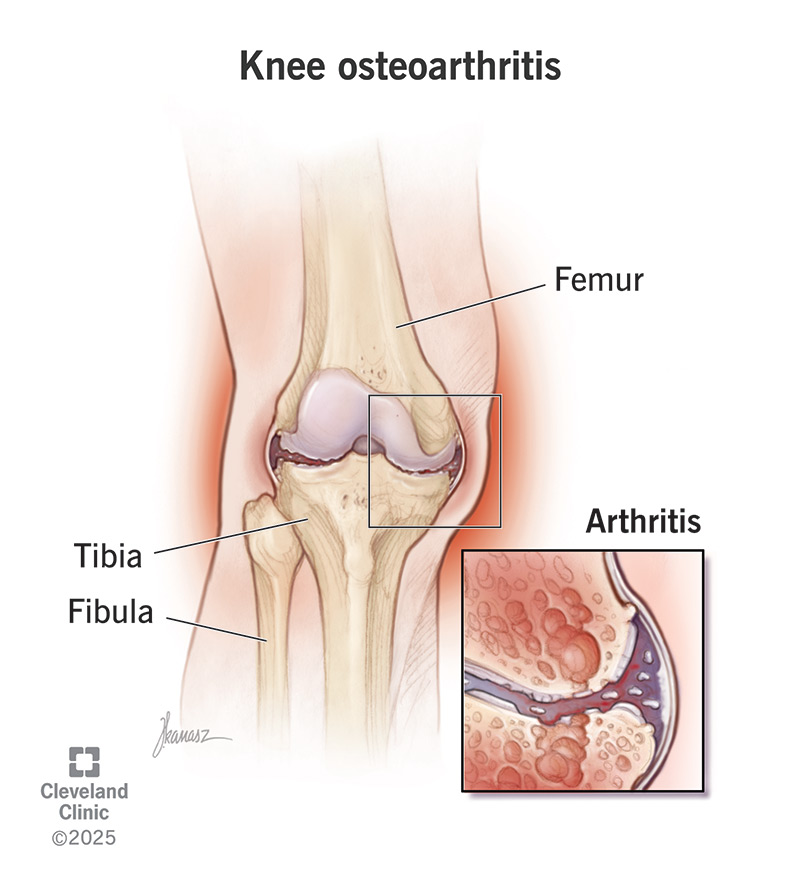
Hand and hip OA
Causes & risk factors
OA develops through a combination of aging, mechanical stress, joint loading, prior injury, genetics, and changes in the cartilage, bone, and soft tissues around the joint. It is not simply a problem of “old cartilage.” Modern understanding views osteoarthritis as a disease of the whole joint, including cartilage, bone, ligaments, and joint lining. Risk rises with age, excess body weight, past trauma, repetitive joint strain, some structural joint differences, and family history in certain patterns such as hand OA.
- Increasing age, especially after midlife
- Excess body weight, especially for knee and hip OA
- Previous joint injury or surgery
- Repetitive joint stress from work, sport, or activity pattern
- Muscle weakness, malalignment, or structural joint issues
- Family tendency in some OA patterns
Evidence-based references (guidelines + high-quality sources)
General patient education: RheumInfo. Clinical overview: NIAMS. Professional review: MSD Manual.
How Osteoarthritis Is Recognized
Osteoarthritis is usually recognized by its typical symptom pattern, the specific joints affected, physical exam findings, and when needed, imaging support. Specialists often look for pain that worsens with use, short-lived stiffness after rest, reduced range of motion, crepitus, bony enlargement, and tenderness over the involved joint. Unlike inflammatory arthritis, OA is less likely to cause prolonged early-morning stiffness, marked warmth, or major systemic symptoms.
Joint pain that worsens with use
Morning or rest stiffness usually under 30 minutes
Crepitus, tenderness, or reduced motion on exam
Bony enlargement or joint shape change over time
Imaging changes consistent with osteoarthritis when needed
Comorbidities & whole-body impact
Osteoarthritis is not only a cartilage problem. Chronic pain from OA can affect sleep, mood, activity level, muscle strength, walking ability, independence, and overall quality of life. Some patients become less active because of pain, which can worsen weight gain, deconditioning, balance problems, and function over time. High-quality OA care looks beyond the joint image alone and focuses on mobility, strength, pain control, and preserving participation in daily life.
- Reduced walking tolerance or slower mobility
- Sleep disruption due to persistent pain
- Muscle weakness around the affected joint
- Lower activity level and physical deconditioning
- Weight gain related to pain-limited activity
- Mood effects such as frustration, low mood, or reduced confidence in movement
Prognosis (what to expect long-term)
OA is usually a long-term condition, but the pace of progression varies widely from person to person. Some patients remain stable for years with manageable symptoms, while others develop worsening pain, stiffness, loss of motion, and reduced function over time. The goal is to control pain early, improve mechanics and strength, reduce unnecessary joint stress, and preserve quality of life for as long as possible.
OA often progresses gradually rather than suddenly.
Many patients improve significantly with weight management, exercise, therapy, and pain-focused treatment.
Advanced cases may eventually need injections or joint replacement depending on the joint and severity.
Understanding Osteoarthritis: Complete Disease Explanation
Osteoarthritis happens when the balance between joint wear, repair, and load tolerance shifts over time. Cartilage becomes less resilient, the joint lining may become irritated, and the bone beneath the cartilage can remodel and form osteophytes. These structural changes alter how the joint moves and absorbs force, which helps explain why OA causes pain, stiffness, swelling, creaking, and progressive loss of easy movement.
What happens at the joint level?
In OA, cartilage no longer cushions the joint as smoothly as before. The surrounding bone may become thicker or form spurs, the joint capsule and lining can become irritated, and nearby muscles may weaken if the joint is used less because of pain. This is why osteoarthritis is best understood as a disease of the entire joint, not just “cartilage wear.”
Joint loading + tissue breakdown → cartilage loss and bone change → pain, stiffness, swelling, and reduced movement over time.
OA vs inflammatory arthritis
Osteoarthritis and inflammatory arthritis can both cause joint pain and stiffness, but they usually behave differently. OA pain is more mechanical, often worse with activity and better with rest, while inflammatory arthritis often causes longer morning stiffness, more swelling, and inflammation-driven symptoms that may improve as the day goes on. Distinguishing between these patterns matters because the treatment approach for osteoarthritis is different from the treatment approach for autoimmune arthritis.
OA usually focuses on exercise, weight management, mechanics, pain relief, and function.
Inflammatory arthritis may require immune-targeting treatment that is not used for routine OA.
Correct classification helps avoid both under-treatment and over-treatment.
Diagnosis: exam, labs, imaging
Osteoarthritis is diagnosed using the overall pattern of symptoms, physical exam findings, and when needed, X-rays or other imaging. Clinicians commonly look at which joints are involved, how the pain behaves, whether stiffness is brief, and whether there is crepitus, tenderness, bony enlargement, or restricted motion. Blood tests are not used to “prove” OA, but they may be ordered to rule out other types of arthritis when symptoms are unclear.
Tests often ordered during initial evaluation
Tests help confirm the pattern, assess severity, and exclude other causes of joint pain when necessary.
- X-rays to look for joint-space narrowing, osteophytes, sclerosis, or other OA changes.
- Blood tests when clinicians need to exclude inflammatory arthritis, gout, or another mimic.
- Focused physical exam to assess pain pattern, joint movement, swelling, strength, and mechanics.
- MRI or other imaging only in selected situations, such as unclear diagnosis or concern for another structural problem.
Treatment: symptom relief + long-term joint care
Effective osteoarthritis treatment has two main goals: reduce current pain and stiffness, and preserve function over the long term. Most patients do best with a layered plan that combines exercise, weight strategies when appropriate, activity modification, physical therapy, and pain-relieving treatment rather than relying on one single intervention. Treatment should be tailored to the joint involved, severity of symptoms, age, activity goals, and overall health.
1) Symptom control (short-term relief)
Short-term relief may include topical treatments, heat or cold, joint supports, exercise adjustment, acetaminophen in selected cases, or nonsteroidal anti-inflammatory drugs when safe. Some patients also benefit from injections, especially when a specific joint such as the knee becomes particularly painful and function-limiting. The safest treatment depends on stomach, kidney, cardiovascular, and bleeding risks as well as other medications the patient may already take.
2) Long-term management (protecting function)
Long-term care focuses heavily on strengthening the muscles that support the joint, improving mechanics, maintaining movement, and reducing unnecessary joint load. For knee and hip OA, weight reduction can meaningfully improve symptoms when excess body weight is a factor. When conservative treatment no longer provides enough relief and function becomes severely limited, joint replacement may become an appropriate option for selected patients.
3) Lifestyle strategies that support treatment
- Use regular low-impact exercise such as walking, cycling, swimming, or structured physical therapy.
- Build muscle strength around the affected joint to improve stability and reduce pain during movement.
- Maintain or work toward a healthier body weight when weight is contributing to knee, hip, or foot symptoms.
- Use pacing and activity modification instead of complete rest, because too little movement can worsen stiffness and weakness.
- Consider braces, footwear changes, walking aids, or ergonomic adjustments when they improve joint mechanics and confidence with movement.
Treatment targets (pain, movement, function)
In osteoarthritis, treatment targets focus on reducing pain, improving joint movement, increasing strength, and preserving everyday function. This means clinicians track not only pain scores, but also walking tolerance, stiffness, sleep, activity level, and whether the patient can still perform important daily tasks. The best outcome is not just “less pain,” but better function with a sustainable plan.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Pain and stiffness | Pain level, flare pattern, morning or rest stiffness | Less discomfort and easier movement through the day |
| Joint function | Walking, stairs, grip, bending, rising from a chair | Better daily activity and more confidence using the joint |
| Long-term mobility | Strength, range of motion, exercise tolerance, sleep impact | Maintained independence and slower functional decline |
Case Study 1 (Example)
Patient developed gradual knee pain with stiffness after activity, worsening over time and improving with rest. Evaluation suggested osteoarthritis rather than ligament- injury or inflammatory arthritis.
Osteoarthritis vs rheumatoid arthritis (quick comparison)
OA and rheumatoid arthritis can both cause pain and stiffness, but they are not the same disease. Osteoarthritis is primarily degenerative and mechanical, while rheumatoid arthritis is an inflammatory autoimmune disease. This difference affects the joints commonly involved, the time-course of stiffness, the presence of swelling and inflammation, and the types of treatment that work best.
| Feature | Osteoarthritis (OA) | Rheumatoid arthritis (RA) |
|---|---|---|
| Main process | Degenerative whole-joint breakdown | Inflammatory autoimmune joint disease |
| Pain pattern | Often worse with use, better with rest | Often associated with inflammatory stiffness and swelling |
| Morning stiffness | Usually under 30 minutes | Often longer and more pronounced |
| Common joints | Knees, hips, hands, spine | Often small joints of hands and feet in a symmetric pattern |
| Testing | X-ray pattern and clinical exam are often key | Inflammatory labs and autoimmune features may be present |
When to seek urgent care
- Hot, very swollen joint with fever or severe illness, because infection must be ruled out urgently.
- Sudden inability to bear weight after injury or abrupt severe joint pain that suggests fracture or another acute structural problem.
- New major redness, warmth, or swelling that seems very different from usual OA symptoms.
- Rapid neurologic symptoms, severe weakness, or bowel/bladder changes when neck or spine symptoms are involved.
Call Now for Osteoarthritis Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My knee and hip pain kept limiting everything I did. The team explained what OA is and gave me a treatment plan that actually helped me move better.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
FAQ
Conclusion
Osteoarthritis is a common and treatable long-term joint disease that can strongly affect pain, movement, sleep, and daily function if symptoms are not addressed early. If you have recurring knee, hip, hand, or spine pain with short-lived stiffness and activity-related worsening, a rheumatology or musculoskeletal evaluation can help clarify the diagnosis and next steps.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always consult with your existing healthcare provider before starting new treatments.
© 2026 Rheumatology Care Associates. All rights reserved.