Medically reviewed by Dr. Priya Prakash (Rheumatologist, board certified) | Last updated: March 20, 2026
What Is Enteropathic Arthritis? Symptoms, Causes, Diagnosis & Treatment
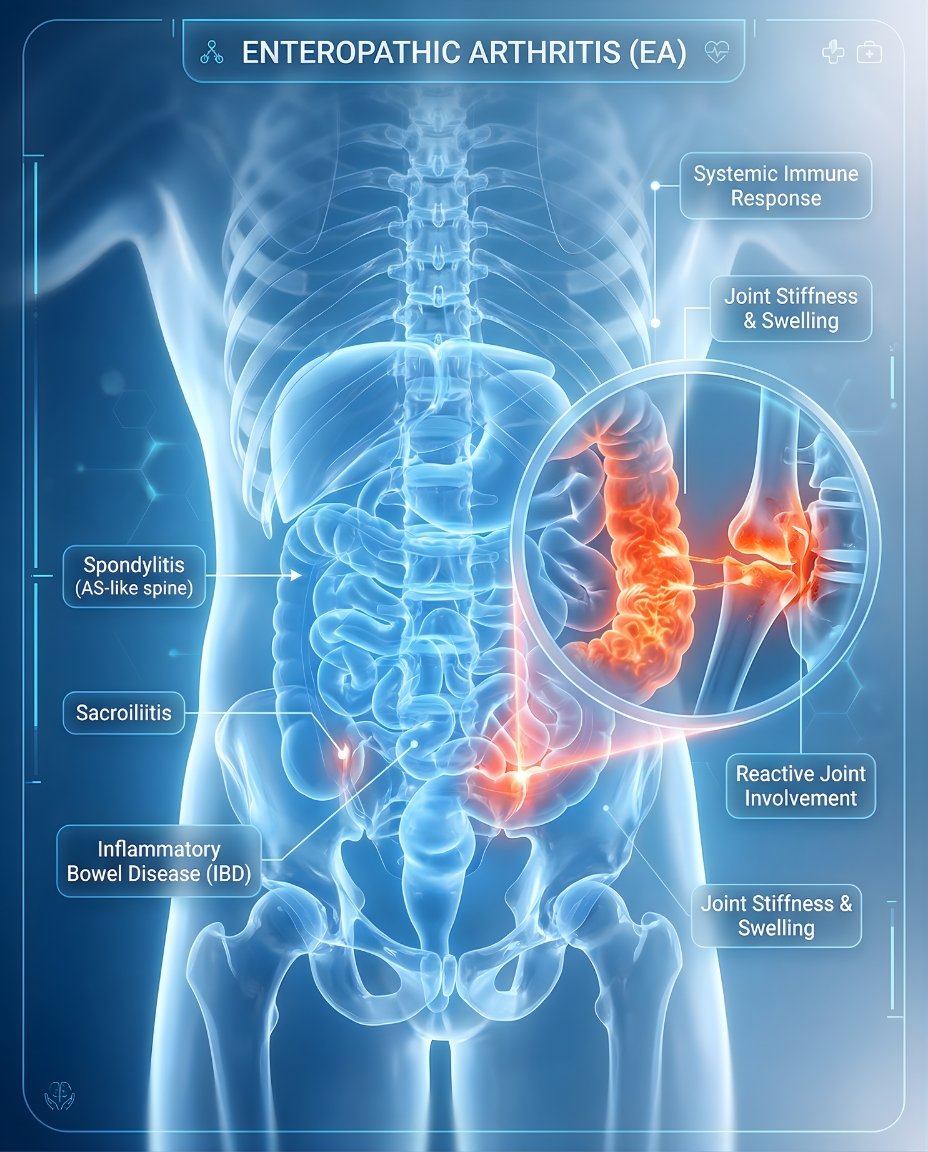
Enteropathic arthritis is an inflammatory arthritis linked to inflammatory bowel disease (IBD), especially Crohn’s disease and ulcerative colitis. It can affect the joints in the arms or legs, the spine, or both, and symptoms may flare along with bowel inflammation in some patients. Early diagnosis and treatment can reduce pain, protect mobility, and help control both joint and gut inflammation.
If you’re searching what is enteropathic arthritis, the simplest answer is that it is arthritis associated with inflammatory bowel disease. Some people develop bowel symptoms first and later notice joint pain or stiffness, while others are evaluated for arthritis before IBD becomes clear. A rheumatologist can confirm the arthritis pattern and help build an individualized enteropathic arthritis treatment plan with attention to both joints and the gut.
Many people notice pain and swelling in the knees, ankles, or other lower-limb joints, though the spine and sacroiliac joints may also be involved. Symptoms can include morning stiffness, back pain, bowel flares, fatigue, and sometimes enthesitis or other spondyloarthritis features. Because treatment choices must consider both bowel disease and joint disease, getting the diagnosis right matters.
Table of Contents
- What Is Enteropathic Arthritis? Simple medical definition
- Enteropathic arthritis at a glance
- Clinical patterns of enteropathic arthritis
- Enteropathic arthritis symptoms (what it feels like)
- Causes & risk factors
- How enteropathic arthritis is recognized
- Comorbidities & whole-body risk
- Prognosis (what to expect long-term)
- Understanding enteropathic arthritis: complete disease explanation
- Enteropathic arthritis vs other spondyloarthritis
- Diagnosis: exam, labs, imaging
- Treatment: symptom relief + disease control
- Treatment targets (joints + bowel control)
- Enteropathic arthritis vs rheumatoid arthritis (quick table)
- When to seek urgent care
- Downloadable enteropathic arthritis symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Enteropathic Arthritis? Simple Medical Definition
Enteropathic arthritis is an inflammatory arthritis associated with inflammatory bowel disease, especially Crohn’s disease and ulcerative colitis. In short, clinically, what is enteropathic arthritis? It is a type of spondyloarthritis that can affect peripheral joints, the sacroiliac joints, and sometimes the spine, while occurring alongside chronic bowel inflammation.
Enteropathic Arthritis at a Glance
IBD link Commonly associated with Crohn’s disease or ulcerative colitis
Peripheral arthritis Knees, ankles, and other limb joints may flare
Axial symptoms Low back or sacroiliac pain may occur
Bowel symptoms Diarrhea, abdominal pain, or bloody stool may coexist
Inflammatory pattern Morning stiffness, swelling, warmth, or flares
Joint symptoms and bowel symptoms may rise together in some patients, but not always.
Clinical Patterns of Enteropathic Arthritis
Enteropathic arthritis can look different from person to person. Clinicians often think about whether the disease mainly affects peripheral joints, the spine, or both, and whether joint flares track with bowel activity.
Peripheral oligoarthritis A few joints, often lower limbs, may flare with IBD activity
Chronic polyarthritis More joints can be involved for longer periods
Axial disease Sacroiliac joints or spine may be affected
Enthesitis pattern Pain where tendons attach to bone may occur
Mixed presentation Some patients have both bowel and musculoskeletal flares
Enteropathic arthritis symptoms (what it feels like)
Typical enteropathic arthritis symptoms include joint pain, swelling, stiffness, and tenderness in the arms or legs, especially the lower limbs. Some patients also have inflammatory back pain, morning stiffness, or sacroiliac symptoms. Because it is linked to bowel inflammation, symptoms may also include abdominal pain, diarrhea, blood in the stool, fatigue, or weight loss depending on the IBD pattern.
Knees • Ankles • Feet • Hips • Low back/SI joints • Abdomen/GI tract • Heel/enthesis areas
IBD
Immune activity
Bowel + joints
Sometimes spine
Pain, stiffness
Bowel flares
Confirm pattern
Treatment plan
Wheel shows a simplified pathway: IBD-related inflammation → joint and bowel symptoms → evaluation and long-term control.
Images for patient education
Joint inflammation
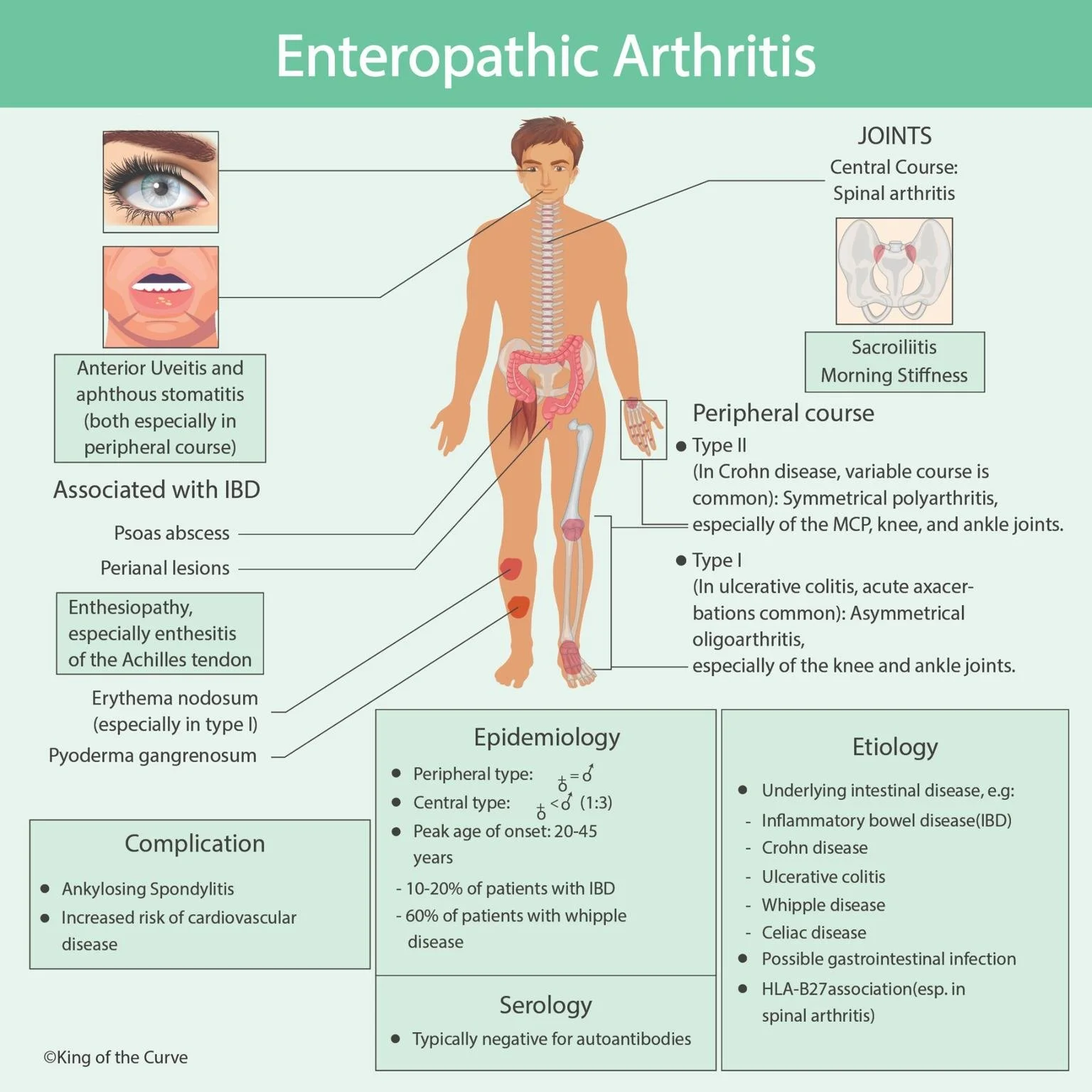
Gut and joint link
Symptom areas
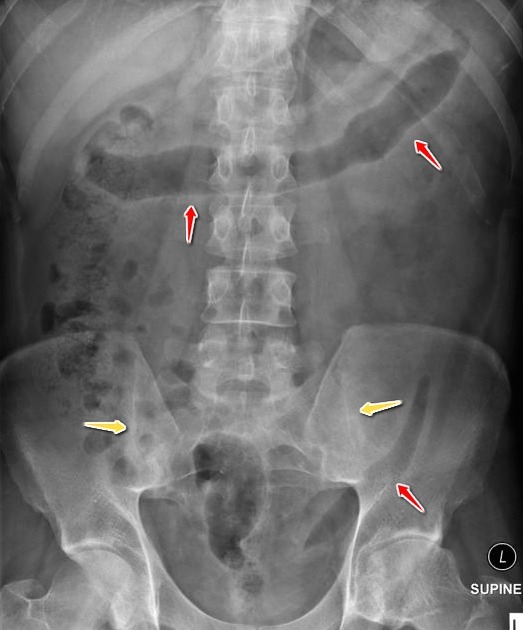
Causes & risk factors
Enteropathic arthritis is driven by immune-system inflammation linked to gastrointestinal disease, especially Crohn’s disease and ulcerative colitis. Not everyone with IBD develops arthritis, but the conditions are closely connected within the broader spondyloarthritis family. In some patients, joint symptoms flare with bowel activity, while in others the arthritis behaves more independently.
- Known Crohn’s disease or ulcerative colitis
- Joint pain, swelling, or morning stiffness
- Lower-limb arthritis or sacroiliac pain
- Bowel flares, abdominal pain, or diarrhea
- Enthesitis or other spondyloarthritis features
Evidence-based references (guidelines + high-quality sources)
General patient education: RheumInfo. Clinical overview: Cleveland Clinic. Review article: PMC review on IBD and enteropathic arthritis.
How Enteropathic Arthritis Is Recognized
Enteropathic arthritis is recognized using the overall pattern of inflammatory joint symptoms plus underlying gastrointestinal disease. Specialists look for the link to IBD, the distribution of joint involvement, possible axial disease, enthesitis, and whether symptoms rise with bowel flares.
Known inflammatory bowel disease
Peripheral joint inflammation, often in lower limbs
Possible sacroiliac or spinal involvement
Inflammatory pattern with stiffness and swelling
Relationship between arthritis and bowel flares in some patients
Comorbidities & whole-body risk
Enteropathic arthritis is not only a joint disease. Patients may also have ongoing bowel inflammation, nutritional stress, fatigue, uveitis, skin findings, or reduced mobility depending on disease pattern. High-quality care looks at both the musculoskeletal and gastrointestinal parts of the disease together.
- Active IBD symptoms such as abdominal pain or diarrhea
- Uveitis or other extraintestinal inflammatory features
- Low back or sacroiliac involvement
- Fatigue and reduced physical function
- Nutritional effects related to bowel disease
- Functional limitation during flares
Prognosis (what to expect long-term)
Enteropathic arthritis is usually a long-term inflammatory condition, but the course varies depending on whether symptoms are mainly peripheral, axial, or tied closely to IBD activity. Some patients have intermittent flares, while others have more persistent bowel and joint disease. The goal is to control inflammation early so joints, mobility, and bowel health are protected as much as possible.
Early treatment can improve pain, stiffness, and function.
Good bowel control can help joint symptoms in some patients.
Many patients do better with coordinated rheumatology and GI care.
Understanding Enteropathic Arthritis: Complete Disease Explanation
Enteropathic arthritis happens when immune-system inflammation associated with inflammatory bowel disease affects the joints, and sometimes the spine or tendon attachment sites. Over time, uncontrolled inflammation can contribute to pain, swelling, stiffness, fatigue, and reduced function. A full evaluation usually looks at the bowel disease pattern along with the arthritis pattern.
What happens at the tissue level?
In enteropathic arthritis, inflammation affects both the gastrointestinal tract and the musculoskeletal system. This helps explain why a patient may have bowel symptoms, joint swelling, back pain, or heel pain as part of the same inflammatory process.
IBD-related immune inflammation → bowel and joint involvement → pain, stiffness, swelling → ongoing symptoms without control.
Enteropathic arthritis vs other spondyloarthritis
Enteropathic arthritis belongs to the spondyloarthritis family along with ankylosing spondylitis and psoriatic arthritis. What makes it different is the clear connection to inflammatory bowel disease, even though the joint pattern can overlap with other inflammatory arthritis types.
Some treatments help both the bowel disease and the arthritis, while others may worsen GI symptoms.
Correct classification helps match therapy to both the joint and intestinal pattern.
Diagnosis: exam, labs, imaging
Enteropathic arthritis is diagnosed using the overall pattern: symptoms, bowel disease history, physical exam, inflammatory markers, and imaging when needed. Clinicians may assess peripheral joints, sacroiliac joints, spinal symptoms, and bowel disease status together.
Tests often ordered during initial evaluation
Tests help support the diagnosis, assess inflammation, and guide safe treatment planning.
- Inflammation markers such as ESR and CRP.
- Assessment of Crohn’s disease or ulcerative colitis activity.
- X-rays or MRI when sacroiliac or spinal involvement is suspected.
- Routine blood tests before certain medications.
Treatment: symptom relief + disease control
Effective enteropathic arthritis treatment has two main goals: reduce joint inflammation and control the underlying bowel disease. Treatment often needs coordination between rheumatology and gastroenterology because the best therapy should help joints without worsening the gut, and some biologic treatments can help both.[web:37][web:42][web:50]
1) Symptom control (short-term relief)
Short-term relief may include local injections, cautious use of pain-relieving strategies, and temporary anti-inflammatory treatment when appropriate. Medication choices must consider bowel disease activity because some options can aggravate gastrointestinal symptoms.[web:37][web:41][web:50]
2) Disease control (preventing progression)
If disease is persistent or active, long-term therapy may include DMARDs or biologic treatment, especially when both bowel and joint inflammation need ongoing control.[web:37][web:40][web:42][web:43] Treatment selection depends on whether symptoms are mainly peripheral, axial, or closely tied to IBD activity.[web:42][web:43]
3) Lifestyle strategies that support treatment
- Stay as active as possible with low-impact movement and stretching.[web:37][web:41]
- Work on posture and mobility if spinal symptoms are present.[web:37][web:41][web:44]
- Stop smoking if applicable, because it can worsen inflammatory outcomes and bowel disease.[web:37]
- Track both bowel flares and joint flares to help guide treatment decisions.[web:36][web:42]
Treatment targets (joints + bowel control)
In enteropathic arthritis, treatment targets focus on lowering inflammation in both the joints and the gastrointestinal tract.[web:36][web:37][web:42] This means clinicians track pain, stiffness, swelling, mobility, bowel symptoms, and whole-body function over time.[web:37][web:42]
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Peripheral joints | Swelling, pain, tenderness, daily function | Less pain and easier movement |
| Axial symptoms | Low back pain, stiffness, posture, mobility | Better flexibility and less stiffness |
| Bowel disease | Diarrhea, abdominal pain, GI flares | Better gut control and fewer flares |
Case Study 1 (Example)
Patient with a history of chronic bowel issues developed joint pain and stiffness, especially in the knees and ankles. Evaluation suggested enteropathic arthritis rather than general- joint pain or overuse injury.
Enteropathic arthritis vs rheumatoid arthritis (quick comparison)
Enteropathic arthritis and rheumatoid arthritis can both cause swollen painful joints, but enteropathic arthritis is more strongly linked to inflammatory bowel disease and may involve the spine or sacroiliac joints.[web:37][web:38][web:42] Rheumatoid arthritis more classically causes symmetric small-joint synovitis without the same bowel-disease connection.[web:37][web:38]
| Feature | Enteropathic arthritis | Rheumatoid arthritis (RA) |
|---|---|---|
| Main association | Inflammatory bowel disease | Autoimmune synovitis without IBD link |
| Joint pattern | Often lower limbs; may involve spine/SI joints | Small peripheral joints more typical |
| Bowel symptoms | May occur with Crohn’s or ulcerative colitis | Not a defining feature |
| Axial disease | Can occur | Less typical |
When to seek urgent care
- Severe abdominal pain, heavy GI bleeding, dehydration, or worsening bowel symptoms.[web:37][web:42]
- Hot, very swollen joint with fever or severe illness, because infection must be ruled out urgently.[web:37]
- Red painful eye, light sensitivity, or blurry vision suggesting possible uveitis.[web:42]
- New neurologic symptoms, severe back symptoms, or sudden major worsening.[web:37][web:42]
Call Now for Enteropathic Arthritis Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My joint pain kept flaring with my bowel symptoms. The team explained what was happening and helped me get better control.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Enteropathic arthritis is a treatable inflammatory arthritis linked to inflammatory bowel disease, and it is often easier to manage when recognized early.[web:36][web:37][web:42] If you have recurring joint pain, morning stiffness, back pain, or bowel flares that seem connected, a rheumatology evaluation can help clarify the diagnosis and next steps.[web:36][web:37]
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always consult with your existing healthcare provider before starting new treatments. Dr. Priya Prakash and Rheumatology Care Associates are committed to evidence-based, personalized care.
© 2026 Rheumatology Care Associates. All rights reserved.