Medically reviewed by Dr. Priya Prakash (Rheumatologist, board certified) | Last updated: March 20, 2026
What Is Dermatomyositis (DM)? Symptoms, Causes, Diagnosis & Treatment
Dermatomyositis (DM) is a rare inflammatory autoimmune disease that affects the muscles and skin. It often causes progressive muscle weakness, especially in the shoulders and hips, along with a characteristic rash on the eyelids, knuckles, chest, or other sun-exposed areas. Early diagnosis and treatment can improve strength, protect daily function, and reduce complications.
If you’re searching what is dermatomyositis, the simplest answer is that DM is an inflammatory muscle disease that usually causes weakness more than pain, along with a visible rash. Many patients notice trouble climbing stairs, rising from a chair, lifting the arms, or carrying objects overhead. A rheumatologist can confirm DM and create an individualized dermatomyositis treatment plan based on symptoms, exam, labs, imaging, and sometimes biopsy.
Myositis
Many people first notice a rash around the eyelids or on the knuckles, followed by gradually worsening weakness in the upper arms or thighs. DM can also affect swallowing, the lungs, energy level, and daily function in some patients. Because symptoms can overlap with other muscle disorders or autoimmune diseases, getting the diagnosis right matters.
Table of Contents
- What Is Dermatomyositis? Simple medical definition
- DM at a glance
- Clinical patterns of dermatomyositis
- Dermatomyositis symptoms (what it feels like)
- Causes & risk factors
- How DM is recognized
- Comorbidities & whole-body risk
- Prognosis (what to expect long-term)
- Understanding DM: complete disease explanation
- DM vs polymyositis
- Diagnosis: exam, labs, imaging
- Treatment: symptom relief + disease control
- Treatment targets (strength and control)
- Dermatomyositis vs lupus (quick table)
- When to seek urgent care
- Downloadable DM symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Dermatomyositis? Simple Medical Definition
Dermatomyositis (DM) is a rare inflammatory autoimmune disease that affects skeletal muscles and skin. In short, clinically, what is DM? It’s an inflammatory myopathy that often causes symmetric muscle weakness and a characteristic rash, and it may also involve the lungs, swallowing muscles, or other organs in some patients.
DM at a Glance
Muscle weakness Often affects shoulders, hips, thighs, and upper arms
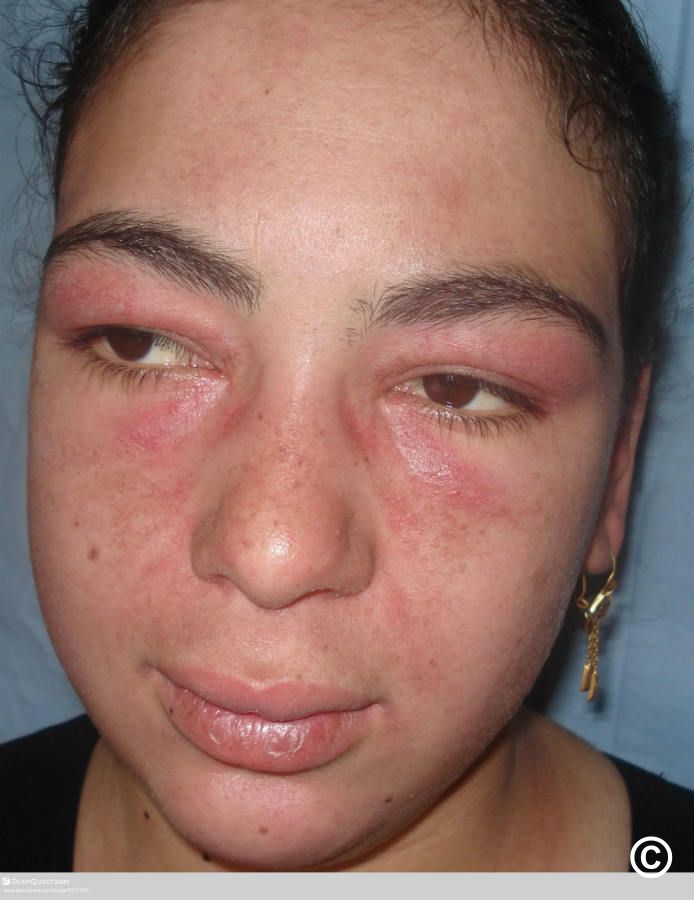
Heliotrope rash Purple or dusky rash around the eyelids
Gottron lesions Rash or bumps over knuckles, elbows, or knees
Fatigue / swallowing issues May occur in more active disease
Sun-sensitive rash Chest, upper back, face, or shoulders may be involved
Symptoms may develop gradually, and weakness often affects daily tasks before pain becomes the main complaint.
Clinical Patterns of Dermatomyositis
Dermatomyositis can look different from person to person. Clinicians often think about whether skin and muscle symptoms occur together, whether the muscle weakness is prominent, and whether complications such as lung disease or swallowing difficulty are present.
Classic dermatomyositis Typical rash plus muscle weakness
Skin-predominant disease Rash may be more obvious than weakness early on
Systemic involvement Lungs, swallowing muscles, or fatigue may be affected
Calcinosis pattern Calcium deposits can occur in some patients, especially children
Persistent active disease Ongoing inflammation can weaken muscles over time
Dermatomyositis symptoms (what it feels like)
Typical dermatomyositis symptoms include progressive muscle weakness, fatigue, and a characteristic rash. Many people notice difficulty climbing stairs, standing from a seated position, lifting the arms, or carrying objects. The rash may appear around the eyes, on the knuckles, elbows, knees, chest, or upper back, and some patients also develop swallowing trouble or shortness of breath.
Eyelids • Knuckles • Elbows • Knees • Chest/V-sign • Upper back/shawl area • Shoulders/hips/thighs
Autoimmunity
Immune triggers
Muscles
Skin rash
Weakness
Fatigue
Confirm diagnosis
Treatment plan
Wheel shows a simplified pathway: immune risk → skin and muscle inflammation → symptoms → evaluation and long-term control.
Images for patient education
DM rash signs
DM muscle weakness
DM symptom areas

Causes & risk factors
DM is considered an autoimmune inflammatory myopathy, meaning the immune system wrongly targets muscles and skin. The exact cause is not fully understood, and risk is likely influenced by immune, genetic, and environmental factors. In adults, dermatomyositis also deserves careful evaluation because it can sometimes be associated with underlying malignancy.
- Progressive weakness in shoulders or hips
- Rash on eyelids, knuckles, chest, or upper back
- Elevated muscle enzymes or abnormal muscle tests
- Swallowing trouble, fatigue, or shortness of breath
- Autoimmune background or related inflammatory features
Evidence-based references (guidelines + high-quality sources)
General patient education: RheumInfo. Clinical overview: NIH/NCBI StatPearls. Diagnosis and testing overview: Mayo Clinic.
How DM Is Recognized
Dermatomyositis is recognized using the overall pattern of characteristic rash, muscle weakness, lab abnormalities, and supportive testing. Specialists often look for proximal symmetric weakness, elevated muscle enzymes, myositis-related autoantibodies, skin findings, MRI or EMG changes, and sometimes biopsy confirmation.
Symmetric proximal muscle weakness
Characteristic skin rash such as heliotrope rash or Gottron lesions
Elevated muscle enzymes on blood tests
Supportive MRI, EMG, skin biopsy, or muscle biopsy findings
Possible lung, swallowing, or systemic involvement
Comorbidities & whole-body risk
Dermatomyositis is not only a skin-and-muscle disease. Some patients also have interstitial lung disease, swallowing problems, calcinosis, or increased cancer risk depending on age and subtype. Good care includes screening for complications and monitoring function beyond the rash alone.
- Interstitial lung disease or breathing symptoms
- Swallowing difficulty or aspiration risk
- Calcinosis in some patients, especially juvenile disease
- Fatigue and reduced physical function
- Skin sensitivity and persistent rash activity
- Malignancy screening considerations in adults
Prognosis (what to expect long-term)
DM is usually a long-term inflammatory disease, but outcomes vary depending on severity, organ involvement, and how quickly treatment begins. Some patients respond well and recover substantial strength, while others need prolonged treatment and monitoring. The goal is to control inflammation early, protect muscle function, and watch for systemic complications.
Early treatment can improve weakness, skin symptoms, and daily function.
Without good control, inflammation can lead to persistent weakness or complications.
Many patients do better with medication, rehabilitation, and regular follow-up.
Understanding DM: Complete disease explanation
Dermatomyositis happens when immune-system inflammation affects muscles and skin, and in some patients also affects lungs or swallowing muscles. Over time, uncontrolled inflammation can cause worsening weakness, fatigue, rash activity, and functional decline. A complete evaluation looks beyond the skin alone because the disease can affect multiple body systems.
What happens at the tissue level?
In DM, inflammation damages muscle tissue and contributes to the distinctive skin findings seen on the eyelids, knuckles, chest, or upper back. This helps explain why people may notice weakness in daily tasks before they think of it as a muscle disease.
Immune dysfunction → muscle and skin inflammation → weakness and rash → possible systemic complications without control.
DM vs polymyositis
Dermatomyositis and polymyositis are both inflammatory muscle diseases, but DM is distinguished by its characteristic skin rash. Both can cause weakness, but the visible rash in dermatomyositis often provides an important clue that helps guide diagnosis.
The rash pattern can help identify dermatomyositis earlier.
Correct classification helps guide testing, complication screening, and long-term management.
Diagnosis: exam, labs, imaging
DM is diagnosed using the overall pattern: symptoms, physical exam, muscle enzyme testing, autoantibodies, and supportive imaging or biopsy. There is no single test that explains every case, so clinicians often combine blood tests with MRI, EMG, skin biopsy, or muscle biopsy when needed.
Tests often ordered during initial evaluation
Tests help support the diagnosis, measure inflammation, and identify complications.
- Muscle enzymes such as CK and related blood markers.
- Autoantibody testing to look for myositis-related immune patterns.
- MRI and sometimes EMG to assess muscle inflammation.
- Skin biopsy or muscle biopsy when confirmation is needed.
Treatment: symptom relief + disease control
Effective dermatomyositis treatment has two main goals: reduce active inflammation now, and preserve strength, swallowing, lung function, and daily activity over time. Standard care often includes immunosuppressive treatment plus rehabilitation and skin protection strategies.
1) Symptom control (short-term relief)
Short-term relief may include anti-inflammatory treatment and skin-directed measures to reduce rash symptoms and weakness burden. The exact approach depends on disease severity, lung involvement, swallowing issues, and medication safety factors.
2) Disease control (preventing progression)
If DM is active or function-limiting, long-term therapy may include corticosteroids and other immunomodulating or immunosuppressive medicines. Treatment choices depend on muscle weakness severity, skin activity, autoantibody pattern, and organ involvement such as lung disease.
3) Lifestyle strategies that support treatment
- Use guided physical therapy to rebuild strength and protect function.
- Protect the skin from sun exposure, which may worsen rash activity.
- Report swallowing trouble, new cough, or breathing symptoms promptly.
- Prioritize rest, pacing, and recovery during active inflammation.
Treatment targets (strength and control)
In DM, treatment targets focus on lowering inflammation, improving muscle strength, controlling the rash, and protecting organ function. This means clinicians track strength, muscle enzymes, skin activity, and whole-body symptoms over time.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Muscle strength | Rising from chair, climbing stairs, arm strength | Improved daily function and endurance |
| Skin activity | Rash color, spread, irritation, sun sensitivity | Less active rash and better comfort |
| Systemic involvement | Lungs, swallowing, fatigue, labs | Better overall disease control |
Case Study 1 (Example)
Patient developed progressive muscle weakness along with a reddish-purple rash over the eyelids and knuckles. Evaluation suggested dermatomyositis rather than skin- allergy or simple muscle fatigue.
Dermatomyositis vs lupus (quick comparison)
DM and lupus can both cause rash and systemic inflammation, but dermatomyositis more classically causes progressive proximal muscle weakness with characteristic rash patterns such as heliotrope rash or Gottron lesions. Lupus may cause rash and fatigue too, but the muscle pattern and diagnostic workup are often different.
| Feature | Dermatomyositis (DM) | Lupus |
|---|---|---|
| Main pattern | Muscle weakness plus characteristic rash | Systemic autoimmune disease with broader organ patterns |
| Skin clues | Heliotrope rash, Gottron lesions, shawl/V-sign | Malar rash and photosensitivity are more typical |
| Muscle symptoms | Proximal weakness is common | Muscle pain can occur, but classic myopathy is less defining |
| Testing focus | Muscle enzymes, myositis antibodies, MRI/biopsy | ANA profile, organ involvement, lupus-specific markers |
When to seek urgent care
- New trouble swallowing, choking, or inability to keep food or liquids down.
- Shortness of breath, worsening cough, or chest symptoms.
- Rapidly worsening weakness affecting walking, standing, or lifting the arms.
- Severe rash change, dehydration, or sudden major worsening that needs urgent evaluation.
Call Now for Dermatomyositis Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My rash and weakness kept getting worse. The team explained what DM is, reviewed my options, and helped me feel stronger.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Dermatomyositis is a treatable inflammatory autoimmune disease that affects muscles and skin, and it is often easier to control when recognized early. If you have progressive weakness, rash around the eyes or knuckles, swallowing difficulty, or unexplained fatigue with muscle symptoms, a rheumatology evaluation can help clarify the diagnosis and next steps.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always consult with your existing healthcare provider before starting new treatments. Dr. Priya Prakash and Rheumatology Care Associates are committed to evidence-based, personalized care.
© 2026 Rheumatology Care Associates. All rights reserved.