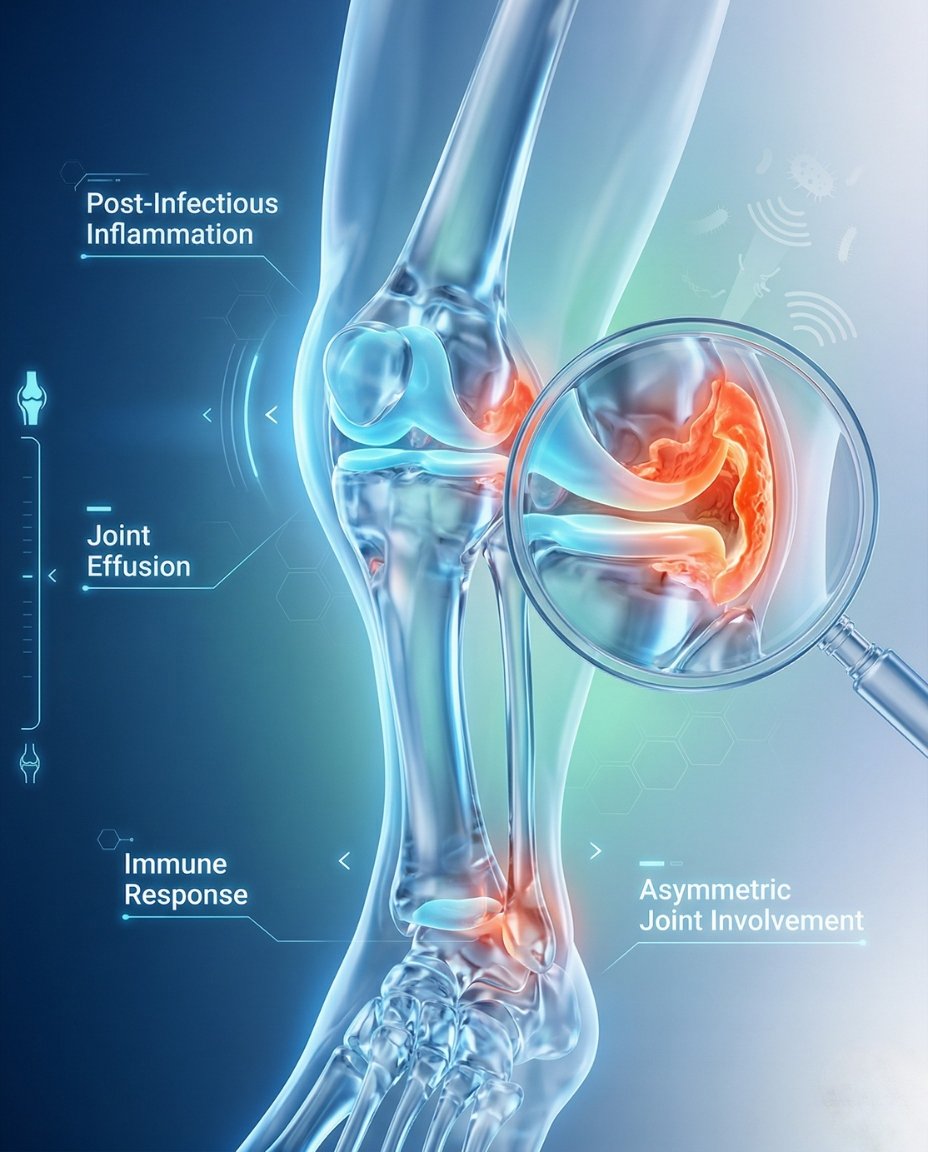
What Is Reactive Arthritis? Symptoms, Causes, Diagnosis & Treatment
Reactive arthritis is an inflammatory arthritis that develops after an infection in another part of the body, most often the bowel, urinary tract, or genital tract. The infection is usually no longer active in the joint itself, but the immune system reacts in a way that causes joint inflammation. It can affect joints, tendons, eyes, skin, and the urinary tract, and early treatment can help reduce pain, swelling, and complications.
If you’re searching what is reactive arthritis, the simplest answer is that it is a form of inflammatory arthritis triggered by a recent infection. Symptoms often begin one to four weeks after the triggering illness and may include swollen painful joints, heel pain, back pain, eye inflammation, urinary symptoms, or skin changes. A rheumatologist can help confirm the diagnosis and create an individualized reactive arthritis treatment plan based on the joints involved, infection history, severity, and whether symptoms are resolving or becoming persistent.
arthritis
Reactive arthritis most often affects the knees, ankles, feet, heels, and sometimes the lower back or sacroiliac joints. It can also cause enthesitis, dactylitis, conjunctivitis, urethritis, mouth ulcers, or rashes on the palms and soles. Because reactive arthritis can overlap with gout, septic arthritis, psoriatic arthritis, inflammatory bowel disease-related arthritis, or other spondyloarthritis conditions, getting the diagnosis right matters.
Table of Contents
- What Is Reactive Arthritis? Simple medical definition
- Reactive arthritis at a glance
- Common reactive arthritis patterns
- Reactive arthritis symptoms (what it feels like)
- Causes & risk factors
- How reactive arthritis is recognized
- Comorbidities & whole-body impact
- Prognosis (what to expect long-term)
- Understanding reactive arthritis: complete disease explanation
- Reactive arthritis vs septic arthritis
- Diagnosis: exam, labs, imaging
- Treatment: symptom relief + long-term management
- Treatment targets (inflammation, function, recurrence)
- Reactive arthritis vs rheumatoid arthritis (quick table)
- When to seek urgent care
- Downloadable reactive arthritis symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Reactive Arthritis? Simple Medical Definition
Reactive arthritis is an inflammatory arthritis in the spondyloarthritis family that appears after certain gastrointestinal or genitourinary infections. In short, clinically, what is reactive arthritis? It is an immune-mediated arthritis triggered by infection elsewhere in the body, often causing asymmetric lower-extremity arthritis, enthesitis, dactylitis, eye inflammation, and sometimes urinary or skin symptoms.
Reactive Arthritis at a Glance
Recent infection Symptoms often begin 1 to 4 weeks after bowel or urinary/genital infection
Lower-body joints Knees, ankles, feet, and heels are common sites
Enthesitis Heel pain or tendon insertion pain is common
Extra-articular symptoms Eyes, skin, mouth, and urinary tract may be involved
Usually acute onset It often starts quickly and can be intense
Not every patient has the classic triad of arthritis, urethritis, and conjunctivitis, so diagnosis depends on the full pattern rather than one textbook picture.
Common Reactive Arthritis Patterns
Reactive arthritis can vary in intensity, duration, and the body areas involved. Some patients mainly have an acute lower-joint arthritis after diarrhea or a urinary/genital infection, while others develop persistent back pain, tendon inflammation, or extra-articular symptoms involving the eyes, skin, or urinary tract. Clinicians often think about reactive arthritis by trigger type, joint pattern, and whether the disease is self-limited or becoming chronic.
Post-GI reactive arthritis Follows bowel infection such as diarrhea illness
Post-GU reactive arthritis Follows urinary or genital infection, often chlamydia-related
Peripheral ReA Knees, ankles, feet, and toes are most affected
Axial ReA Lower back or sacroiliac inflammation becomes prominent
Chronic or relapsing ReA Symptoms persist or recur over time
Reactive arthritis symptoms (what it feels like)
Typical reactive arthritis symptoms include painful swollen joints, stiffness, heel pain, tendon pain, and sometimes lower back pain. Many patients notice that the knees, ankles, feet, or toes become inflamed, warm, stiff, and difficult to use. Some people also develop red or irritated eyes, pain with urination, mouth ulcers, skin changes on the palms or soles, or sausage-like swelling of fingers or toes.
Knees • Ankles • Feet • Heels • Toes • Lower back • Eyes • Urinary tract • Skin
Recent infection
GI or GU source
Post-infectious
Inflammation
Arthritis, enthesitis
Eye or urinary signs
Confirm pattern
Treatment plan
Wheel shows a simplified pathway: infection trigger → immune-driven inflammation → joint and extra-articular symptoms → evaluation and management.
Images for patient education
Lower joint swelling
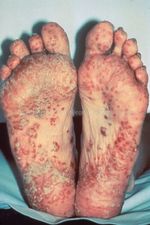
Heel and tendon pain
Eye and urinary symptoms

Causes & risk factors
Reactive arthritis is triggered by an infection, most often in the gastrointestinal or genitourinary tract. Common triggers include infections related to bacteria such as chlamydia, salmonella, shigella, campylobacter, and other bowel or urinary pathogens. Not everyone who gets these infections develops arthritis, which suggests that immune predisposition and genetic factors such as HLA-B27 can influence risk and disease course.
- Recent diarrhea, food-borne illness, or bowel infection
- Recent urinary or genital infection, including STI-related triggers
- Painful swollen joints in the lower body
- Heel pain, enthesitis, or dactylitis
- Eye irritation, urinary symptoms, or skin lesions
- HLA-B27 positivity may increase recurrence or chronic risk
Evidence-based references (guidelines + high-quality sources)
General patient education: RheumInfo. Clinical overview: NIAMS. Professional review: NIH/NCBI StatPearls.
How Reactive Arthritis Is Recognized
Reactive arthritis is recognized through the pattern of symptoms and the history of a recent infection. Specialists often look for acute asymmetric arthritis of the lower limbs, enthesitis, dactylitis, eye inflammation, or urinary symptoms that begin days to weeks after a triggering illness. The diagnosis often depends on connecting the timing of the infection and the inflammatory symptoms, while also excluding other types of arthritis.
Arthritis beginning 1 to 4 weeks after infection
Lower-extremity joint involvement
Enthesitis or heel pain
Conjunctivitis, eye pain, or urinary symptoms
Skin or mouth findings in some patients
Pattern fitting a post-infectious spondyloarthritis
Comorbidities & whole-body impact
Reactive arthritis can affect more than the joints. Tendons, eyes, skin, mucous membranes, the urinary tract, and the lower spine may all be involved, which is why the illness can feel like more than “just arthritis.” Some patients recover fully, while others develop relapsing symptoms, chronic sacroiliac pain, or longer-term inflammatory arthritis.
- Enthesitis or tendon pain, especially at the heel
- Dactylitis with sausage-like swelling of fingers or toes
- Conjunctivitis or other eye inflammation
- Urethritis or urinary discomfort
- Mouth ulcers or skin lesions on palms and soles
- Chronic back pain or sacroiliac involvement in some cases
Prognosis (what to expect long-term)
Reactive arthritis often has a self-limited course, and many patients improve within several months. However, some people develop symptoms lasting longer than six months, recurrent flares, or chronic sacroiliac and peripheral joint involvement. The risk of recurrence and chronic disease may be higher in patients with HLA-B27 positivity or more severe initial disease.
Many cases improve within months.
Some patients have relapses or more persistent symptoms.
Good follow-up matters, especially when back pain, eye inflammation, or chronic joint symptoms continue.
Understanding Reactive Arthritis: Complete Disease Explanation
Reactive arthritis happens when the immune system reacts abnormally after an infection and causes inflammation in the joints and related tissues. The triggering infection is usually in the bowel, urinary tract, or genital tract, not in the joint itself. This is why reactive arthritis is considered a post-infectious inflammatory condition rather than a septic joint infection.
What happens at the body level?
In reactive arthritis, immune activation after infection can target joints, tendon insertions, and other tissues such as the eyes or skin. This helps explain why the disease may involve arthritis, enthesitis, conjunctivitis, urethritis, and skin changes together or in different combinations. The classic triad is well known, but many patients do not present with every feature at the same time.
GI or GU infection → immune reaction after infection → joint and tendon inflammation → arthritis, enthesitis, eye, skin, and urinary symptoms.
Reactive arthritis vs septic arthritis
Reactive arthritis and septic arthritis can both cause a hot swollen joint, but they are very different conditions. Septic arthritis is an infection inside the joint and is a medical emergency, while reactive arthritis is an immune-mediated inflammatory reaction triggered by infection elsewhere in the body. Distinguishing between them is critical because one needs urgent antibiotics and drainage, while the other is treated as an inflammatory arthritis.
Septic arthritis can rapidly destroy a joint and needs urgent treatment.
Reactive arthritis is inflammatory and often treated with anti-inflammatory medication and management of the trigger context.
Joint aspiration may be important when the diagnosis is uncertain.
Diagnosis: exam, labs, imaging
Reactive arthritis is diagnosed using the overall clinical picture, history of infection, physical exam findings, and selected tests. Doctors may ask about recent diarrhea, STI exposure, urinary symptoms, red eyes, mouth sores, or heel pain, then examine the joints, tendons, skin, and eyes. Testing may include joint-fluid analysis to rule out infection or gout, stool or urine testing, inflammatory markers, and imaging when back pain or sacroiliac involvement is suspected.
Tests often ordered during initial evaluation
Tests help support the diagnosis and rule out look-alike conditions.
- History and physical exam focused on recent GI or GU infection, joint pattern, enthesitis, skin, eyes, and urinary symptoms.
- Blood tests such as ESR and CRP to assess inflammation.
- Joint aspiration when a swollen joint needs evaluation for infection, gout, or another cause.
- Urine, stool, or STI-related testing when clinicians are trying to identify a triggering infection.
- X-rays, ultrasound, MRI, or other imaging when chronic changes or sacroiliac involvement are suspected.
Treatment: symptom relief + long-term management
Effective reactive arthritis treatment has two main goals: reduce inflammation and pain, and address the triggering infection context when relevant. NSAIDs are usually first-line treatment for joint inflammation, while corticosteroids, local injections, or DMARDs may be used when symptoms are more severe or persistent. If there is evidence of an active bacterial infection, antibiotics may be appropriate, especially in selected genitourinary trigger settings.
1) Symptom control (short-term relief)
NSAIDs are usually the first treatment for acute reactive arthritis. Some patients also benefit from joint injections or short-term corticosteroid treatment, especially if a particular joint or tendon insertion is very inflamed. Supportive care may include rest during a flare, followed by gradual return to movement and physical therapy when function is limited.
2) Long-term management (persistent or chronic disease)
If symptoms do not settle, longer-term treatment may include DMARDs such as sulfasalazine or methotrexate, and sometimes biologic therapy in more difficult cases. Long-term care also includes treating the consequences of chronic enthesitis, sacroiliac pain, or recurrent flares. The treatment plan depends on how much disease remains after the initial infection-related phase has passed.
3) Lifestyle strategies that support treatment
- Stay active as tolerated, because prolonged immobility can worsen stiffness and functional loss.
- Use physical therapy or guided exercise when heel pain, back stiffness, or lower-limb weakness affects movement.
- Report red painful eyes, vision changes, or severe urinary symptoms promptly.
- Follow through on infection evaluation and treatment recommendations, including STI-related care when relevant.
- Track flare timing, infection history, and which joints or tendons are affected.
Treatment targets (inflammation, function, recurrence)
In reactive arthritis, treatment targets focus on controlling inflammation, restoring movement, preventing persistent tendon and joint pain, and monitoring for recurrence. Clinicians track swollen joints, heel pain, back symptoms, eye symptoms, urinary symptoms, and how well the patient returns to normal walking and daily activity. Good control means less inflammation, better function, and lower risk of chronic disease.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Joint inflammation | Pain, swelling, warmth, stiffness, number of affected joints | Less pain and fewer swollen joints |
| Function | Walking, standing, heel pain, back mobility, daily activity | Improved movement and easier daily function |
| Systemic and relapse control | Eye symptoms, urinary symptoms, recurrence, chronic sacroiliac disease | Stable disease with fewer flares and safer long-term control |
Case Study 1 (Example)
Patient developed joint pain and swelling a few weeks after a gastrointestinal or urinary infection. Evaluation suggested reactive arthritis rather than post- viral weakness or simple joint strain.
Reactive arthritis vs rheumatoid arthritis (quick comparison)
Reactive arthritis and rheumatoid arthritis are both inflammatory, but they behave differently. Reactive arthritis usually follows an infection and often affects lower-extremity joints asymmetrically with enthesitis or eye and urinary symptoms, while rheumatoid arthritis more often causes a chronic symmetric small-joint pattern. This distinction matters because the trigger history, associated features, and long-term treatment approach are different.
| Feature | Reactive arthritis | Rheumatoid arthritis |
|---|---|---|
| Typical trigger | Recent GI or GU infection | No infection trigger required |
| Joint pattern | Often asymmetric, lower-body predominant | Often symmetric, small joints commonly involved |
| Extra features | Eye, urinary, skin, enthesitis, dactylitis | Primarily inflammatory synovitis and systemic autoimmune features |
| Back or sacroiliac involvement | Can occur | Less typical |
| Disease family | Spondyloarthritis | Autoimmune inflammatory polyarthritis |
When to seek urgent care
- Hot swollen joint with fever or severe illness, because septic arthritis must be ruled out urgently.
- Red painful eye, vision changes, or major light sensitivity, because inflammatory eye disease can require urgent treatment.
- Severe urinary symptoms, suspected STI complications, or ongoing infection concerns.
- Rapid worsening, inability to walk, or major swelling that seems different from a typical flare.
Call Now for Reactive Arthritis Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My joint pain started after an infection and I didn’t connect the two. The team explained reactive arthritis clearly and helped me get the right treatment.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Reactive arthritis is a treatable post-infectious inflammatory arthritis that can affect joints, tendons, eyes, skin, and the urinary tract. If you develop joint swelling, heel pain, back pain, or eye and urinary symptoms after a recent infection, a rheumatology evaluation can help clarify the diagnosis and start the right treatment plan.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always seek prompt care for a hot swollen joint, severe eye symptoms, or signs of infection.
© 2026 Rheumatology Care Associates. All rights reserved.