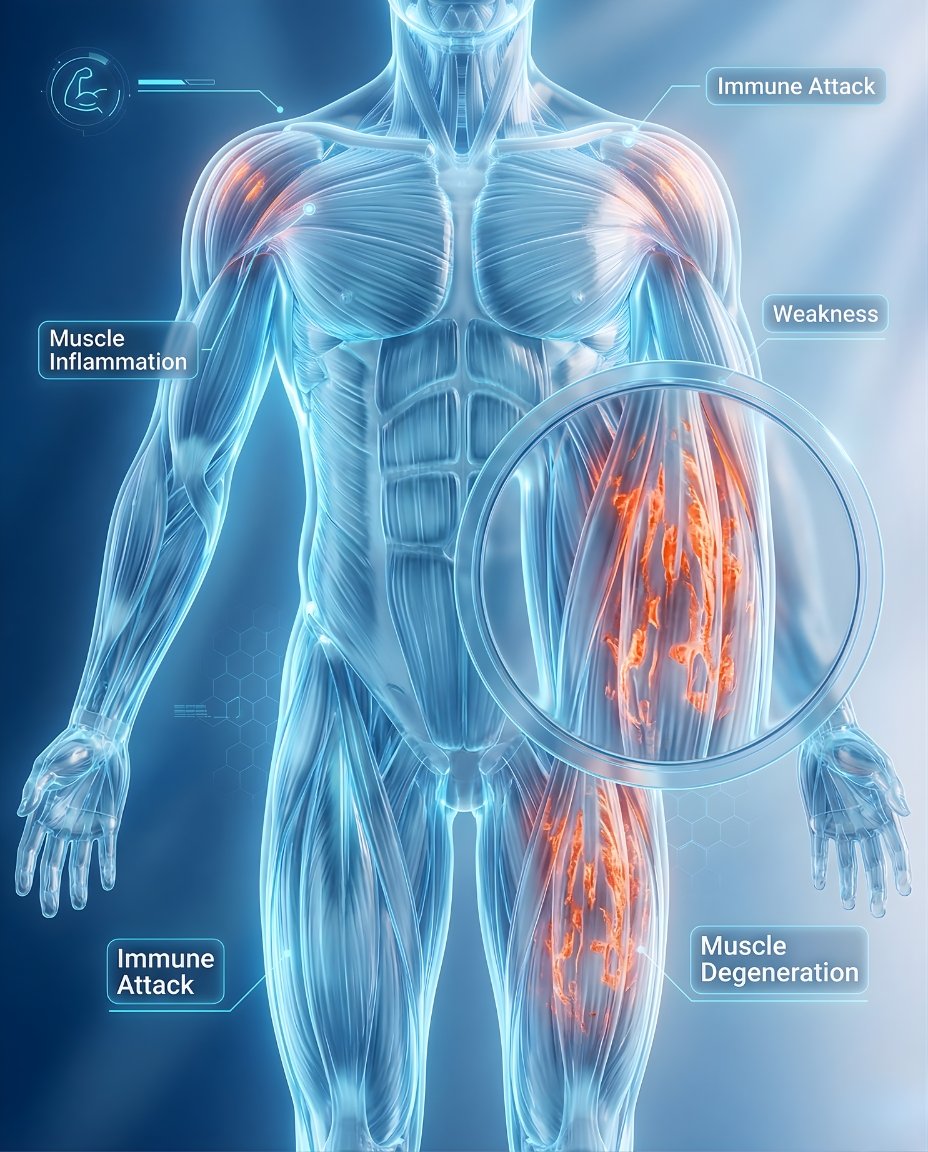
What Is Polymyositis? Symptoms, Causes, Diagnosis & Treatment
Polymyositis is a rare inflammatory autoimmune muscle disease that causes progressive muscle weakness, especially in muscles closest to the trunk such as the shoulders, hips, thighs, neck, and upper arms. Weakness usually develops on both sides of the body and can make climbing stairs, getting up from a chair, lifting the arms, or swallowing difficult. Early diagnosis and treatment can reduce inflammation, preserve muscle function, and help monitor for complications such as swallowing trouble or lung involvement.
If you’re searching what is polymyositis, the simplest answer is that polymyositis is an inflammatory muscle disease in which the immune system attacks skeletal muscles and causes ongoing weakness, especially in proximal muscle groups. Some patients mainly notice leg and shoulder weakness at first, while others also develop fatigue, muscle pain, trouble swallowing, or reduced exercise tolerance. A rheumatologist can help confirm the diagnosis and create an individualized polymyositis treatment plan based on symptoms, strength testing, muscle-enzyme blood work, imaging, and sometimes muscle biopsy.
Myositis
Polymyositis is part of the idiopathic inflammatory myopathy group and usually affects adults rather than children. It can sometimes involve muscles used for swallowing or breathing, and some patients also develop interstitial lung disease. Because polymyositis can overlap with dermatomyositis, inclusion body myositis, thyroid disease, statin-related muscle injury, infection, and other neuromuscular or inflammatory conditions, getting the diagnosis right matters.
Table of Contents
- What Is Polymyositis? Simple medical definition
- Polymyositis at a glance
- Common polymyositis patterns
- Polymyositis symptoms (what it feels like)
- Causes & risk factors
- How polymyositis is recognized
- Comorbidities & whole-body impact
- Prognosis (what to expect long-term)
- Understanding polymyositis: complete disease explanation
- Polymyositis vs dermatomyositis
- Diagnosis: exam, labs, testing
- Treatment: symptom relief + long-term disease control
- Treatment targets (strength, function, complications)
- Polymyositis vs polymyalgia rheumatica (quick table)
- When to seek urgent care
- Downloadable polymyositis symptom checklist
- Related conditions (internal links)
- FAQs
- Conclusion + next steps
What Is Polymyositis? Simple Medical Definition
Polymyositis is a rare inflammatory myopathy characterized by immune-mediated muscle inflammation and progressive weakness, especially in proximal muscles. In short, clinically, what is polymyositis? It is an autoimmune muscle disease in which inflammation affects skeletal muscle fibers, leading to symmetric weakness that often involves the shoulders, upper arms, hips, thighs, and sometimes swallowing muscles.
Polymyositis at a Glance
Proximal muscle weakness Shoulders, hips, thighs, and upper arms are commonly affected on both sides
Gradual progression Weakness often develops over weeks to months rather than overnight
Daily activity impact Climbing stairs, rising from a chair, lifting the arms, or carrying objects may become difficult
Muscle test abnormalities CK and other muscle enzymes are often elevated
Needs specialized workup MRI, EMG, antibody testing, and sometimes muscle biopsy help support diagnosis
Polymyositis usually causes true muscle weakness more than joint-centered pain or morning stiffness.
Common Polymyositis Patterns
Polymyositis can present in more than one way, which is one reason diagnosis may take time. Some patients mainly develop progressive shoulder and hip weakness, while others also have swallowing difficulty, breathing symptoms, fatigue, weight loss, or lung involvement. Clinicians often think about the disease by its severity, rate of progression, and whether there are features suggesting another inflammatory myopathy subtype.
Classic proximal polymyositis Symmetric weakness of shoulder and hip muscles dominates
Bulbar-involved polymyositis Swallowing or choking symptoms become important
Respiratory-involved polymyositis Shortness of breath or lung complications appear
Systemic inflammatory polymyositis Fatigue, low-grade fever, and weight loss accompany weakness
Persistent or relapsing polymyositis Weakness improves partly, then plateaus or returns over time
Polymyositis symptoms (what it feels like)
Typical polymyositis symptoms include progressive weakness in the shoulders, upper arms, hips, thighs, and neck. Many patients notice trouble climbing stairs, standing up from a chair, reaching overhead, lifting objects, or keeping pace with usual daily activity. Some people also develop muscle pain or tenderness, fatigue, trouble swallowing, difficulty speaking clearly, shortness of breath, weight loss, or joint discomfort.
Shoulders • Upper arms • Neck • Hips • Thighs • Swallowing muscles • Breathing • Energy
Autoimmune tendency
Adult onset
Immune attack on
skeletal muscle
Weakness, fatigue
Swallowing issues
Confirm myositis
Protect function
Wheel shows a simplified pathway: immune-mediated muscle inflammation → progressive weakness and function loss → evaluation and long-term disease control.
Images for patient education
Shoulder weakness
Hip and thigh weakness

Function loss
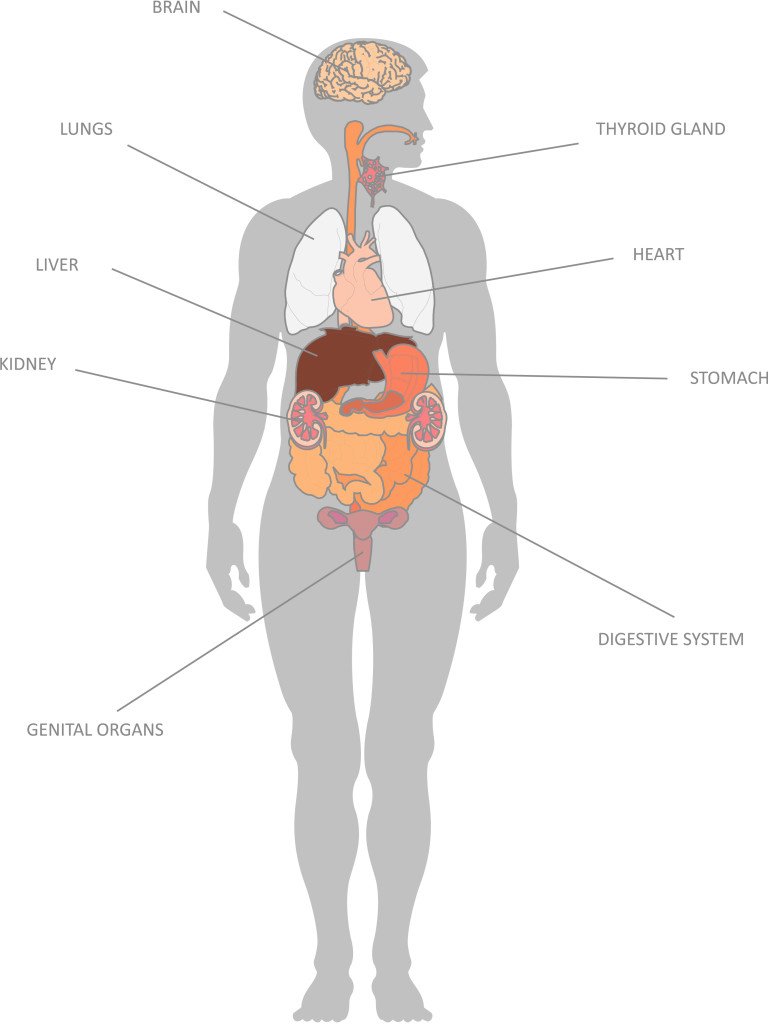
Causes & risk factors
Polymyositis develops because of abnormal immune activity that targets muscle tissue, although the exact trigger is not fully understood. Genetic susceptibility, immune-system dysregulation, and possible environmental or infectious triggers may all contribute in some patients. The disease is not simply due to aging, inactivity, or ordinary muscle strain, even though weakness may initially be mistaken for those problems.
- Autoimmune inflammation affecting skeletal muscle
- Progressive symmetric proximal weakness
- Elevated CK or other muscle enzymes in many patients
- MRI, EMG, antibody, and biopsy-based diagnostic support
- Swallowing symptoms or breathing symptoms in some cases
- Interstitial lung disease risk in part of the inflammatory myopathy population
Evidence-based references (guidelines + high-quality sources)
General patient education: Cleveland Clinic. Clinical overview: Mayo Clinic. Diagnosis and treatment overview: Mayo Clinic.
How Polymyositis Is Recognized
Polymyositis is recognized by the combination of progressive proximal muscle weakness, supportive laboratory findings, and evidence of inflammatory muscle disease on specialized testing. Specialists often look for symmetric shoulder and hip weakness, difficulty climbing stairs or rising from a chair, elevated CK or related muscle enzymes, myopathic findings on EMG, and MRI or biopsy evidence of muscle inflammation. The diagnosis can be challenging because symptoms may overlap with other inflammatory myopathies, medication-related muscle injury, endocrine disorders, neurologic disease, or chronic deconditioning.
Progressive proximal weakness
Symmetric shoulder and hip involvement
Difficulty standing, climbing, or lifting the arms
Elevated CK or other muscle enzymes
Abnormal MRI, EMG, or biopsy findings
Evidence against alternative muscle disorders
Comorbidities & whole-body impact
Polymyositis can affect many parts of daily life because ongoing weakness changes mobility, endurance, independence, swallowing safety, and quality of life. Fatigue, aspiration risk, lung disease, deconditioning, medication side effects, and emotional stress can all influence long-term outcomes. High-quality care requires attention not only to muscle inflammation, but also to function, breathing symptoms, nutritional status, and treatment safety.
- Fatigue and reduced day-to-day stamina
- Trouble swallowing and choking risk in some patients
- Aspiration pneumonia risk when dysphagia is significant
- Interstitial lung disease or respiratory symptoms in some cases
- Muscle deconditioning and reduced function over time
- Side effects from long-term steroid or immunosuppressive therapy
Prognosis (what to expect long-term)
The outlook for polymyositis has improved because of earlier recognition, better immunosuppressive treatment, rehabilitation strategies, and closer follow-up. Even so, long-term outcomes depend on how early treatment begins, how well weakness responds, and whether swallowing or lung complications develop. The central goals are to reduce inflammation, preserve strength, prevent irreversible muscle damage, and protect breathing, nutrition, and quality of life.
Many patients improve with treatment, but recovery often takes time.
Persistent weakness or relapse may require more than steroids alone.
Lung involvement or severe swallowing problems need closer follow-up.
Understanding Polymyositis: Complete Disease Explanation
Polymyositis occurs when the immune system becomes abnormally activated and targets muscle fibers, causing inflammation and muscle injury. This immune-driven process helps explain why the disease mainly affects muscles used for lifting, climbing, standing, and other proximal movements. It also explains why some patients develop swallowing difficulty or respiratory symptoms when the disease involves additional muscle groups or overlaps with lung disease.
What happens at the immune and muscle level?
In polymyositis, inflammatory immune cells enter muscle tissue and contribute to muscle fiber damage. As inflammation continues, muscles may weaken further and daily movements may become harder, even if joint pain is not the main complaint. The final result is a disease that can gradually limit independence unless inflammation is recognized and treated appropriately.
Immune dysregulation → muscle inflammation → muscle fiber injury → proximal weakness → function loss, swallowing issues, or respiratory complications in some patients.
Polymyositis vs dermatomyositis
Polymyositis and dermatomyositis are related inflammatory myopathies, and both can cause proximal muscle weakness. The key difference is that dermatomyositis usually includes characteristic skin findings, while polymyositis is defined by inflammatory muscle disease without the classic dermatomyositis rash pattern. Distinguishing between them matters because antibody patterns, associated risks, and disease classification may differ.
Polymyositis centers on inflammatory muscle weakness without classic dermatomyositis rash.
Dermatomyositis often includes visible skin findings along with muscle disease.
Correct classification helps guide testing, monitoring, and treatment strategy.
Diagnosis: exam, labs, testing
Polymyositis is diagnosed using the overall clinical pattern together with muscle blood tests, physical examination, and targeted neuromuscular evaluation. Doctors often order CK, aldolase, AST, ALT, LDH, ANA, and sometimes myositis-related antibody testing, then combine those results with strength testing, MRI, EMG, and selected biopsy findings. Because inflammatory myopathies can resemble each other and overlap with other disorders, diagnosis often depends on multiple pieces of evidence rather than one single test.
Tests often ordered during initial evaluation
Tests help confirm the diagnosis, define severity, and guide treatment safety.
- Blood tests such as CK, aldolase, AST, ALT, LDH, ANA, and selected myositis-related antibody panels.
- Physical examination focused on proximal strength, neck flexion strength, swallowing symptoms, and functional impairment.
- MRI to identify inflamed muscle areas and help guide biopsy site selection when needed.
- EMG to look for a myopathic pattern that supports inflammatory muscle disease.
- Muscle biopsy in selected cases when tissue confirmation is needed.
Treatment: symptom relief + long-term disease control
Effective polymyositis treatment has two main goals: control active muscle inflammation and preserve or restore strength and function. Corticosteroids are a main early treatment, while steroid-sparing immunosuppressive medicines such as methotrexate or azathioprine are commonly used for longer-term control, and some patients need IVIG or other advanced therapies. Long-term management also includes rehabilitation, complication monitoring, and ongoing reassessment of swallowing, lung symptoms, and medication safety.
1) Symptom control (short-term relief)
Early treatment usually focuses on lowering inflammation quickly enough to reduce further muscle injury and start strength recovery. Patients may notice gradual improvement in function, but recovery is often not as immediate as in some other inflammatory rheumatic conditions. Supportive care during this phase may include physical therapy guidance, fall prevention, swallowing evaluation, and review of breathing symptoms.
2) Long-term management (disease control and organ protection)
Long-term treatment may include corticosteroid tapering, methotrexate, azathioprine, IVIG, or other immunomodulatory therapy depending on severity and response. The main goal is to maintain strength, reduce relapse risk, minimize treatment toxicity, and prevent complications such as aspiration or progressive lung disease. Long-term care also includes regular laboratory monitoring, functional reassessment, and careful review of respiratory or nutritional concerns when present.
3) Lifestyle strategies that support treatment
- Work with guided physical therapy or supervised exercise to rebuild strength safely as inflammation improves.
- Report choking, coughing with meals, unexplained weight loss, or worsening swallowing symptoms promptly.
- Report shortness of breath, persistent dry cough, or declining exercise tolerance because lung involvement may need further evaluation.
- Protect bone health during corticosteroid use with appropriate calcium, vitamin D, and osteoporosis prevention when advised.
- Keep follow-up visits and lab testing because medication adjustment usually depends on both symptoms and objective disease markers.
Treatment targets (strength, function, complications)
In polymyositis, treatment targets focus on improving muscle strength, restoring daily function, and reducing complications related to swallowing, breathing, and treatment toxicity. Clinicians track exam findings, stair climbing, chair rise, arm elevation, swallowing safety, muscle enzymes, and overall function over time. Good control means more than lower inflammation alone; it also means safer eating, better mobility, more independence, and preserved long-term muscle performance.
| Target area | What your clinician tracks | What “on target” can look like |
|---|---|---|
| Muscle strength | Hip and shoulder power, chair rise, stair climbing, arm elevation | Clear improvement in proximal strength and less effort with movement |
| Function and safety | Dressing, walking, lifting, swallowing, fatigue, daily activity tolerance | Better independence and safer everyday activity |
| Complication control | CK trend, steroid side effects, lung symptoms, aspiration risk, relapse signs | Stable disease with safer long-term treatment and preserved function |
Case Study 1 (Example)
Patient developed progressive muscle weakness, especially in the thighs and shoulders, making it difficult to climb stairs or lift objects. Evaluation suggested polymyositis rather than muscle- strain or simple fatigue.
Polymyositis vs polymyalgia rheumatica (quick comparison)
Polymyositis and polymyalgia rheumatica can both limit movement, but they are very different diseases. Polymyositis is an inflammatory muscle disease that causes true muscle weakness, while polymyalgia rheumatica mainly causes pain and marked stiffness around the shoulders and hips, especially in older adults. Distinguishing between them matters because their testing approach, complications, and long-term treatment strategy are different.
| Feature | Polymyositis | Polymyalgia rheumatica (PMR) |
|---|---|---|
| Main mechanism | Inflammatory muscle disease causing proximal weakness | Inflammatory rheumatic syndrome causing pain and stiffness |
| Main complaint | Difficulty climbing, lifting, standing, or swallowing | Morning stiffness, aching, and pain-limited movement |
| Typical testing | CK, MRI, EMG, antibody testing, muscle biopsy | ESR, CRP, symptom pattern, exclusion of mimics |
| Typical age | Usually adult onset | Usually over age 50 |
| Treatment focus | Immune suppression plus function recovery | Low-dose steroids with tapering and symptom monitoring |
When to seek urgent care
- New or worsening trouble swallowing, choking, or coughing during meals.
- Shortness of breath, chest symptoms, rapidly declining exercise tolerance, or suspected lung involvement.
- Rapid severe worsening of weakness, especially if walking, standing, or holding the head up becomes difficult.
- High fever, marked illness, or symptoms suggesting infection, aspiration, or another acute medical problem.
Call Now for Polymyositis Care
⭐ Google Rating: 4.7/5 (184 reviews) • Insurance accepted: Most major plans (verify with office).
Patient testimonial: “My leg and shoulder weakness kept getting worse, and I could not understand why simple movements were getting so hard. The team explained polymyositis clearly and guided the right workup and treatment.”
Call Now: (352) 717-0603 Request AppointmentClinic Address
Rheumatology Care Associates PLLC (RCA)
2611 S US Hwy 27, Clermont, FL 34711
Email: info@rheumatologycareassociates.com
Office hours: Mon 8:30AM–5:00PM; Tue 8:30AM–5:00PM; Wed 8:00AM–3:30PM; Thu 8:30AM–5:00PM; Fri 9:00AM–1:30PM.
Related conditions (internal links)
FAQ
Conclusion
Polymyositis is a serious but treatable inflammatory muscle disease that can affect strength, function, swallowing, and breathing over time. If you have unexplained progressive weakness in the shoulders or thighs, trouble rising from a chair, or new swallowing or breathing symptoms, a rheumatology evaluation can help confirm the diagnosis and build the right long-term treatment plan.
Disclaimer: This article is for educational purposes and does not replace professional medical advice. Always seek prompt care for trouble swallowing, shortness of breath, chest symptoms, or rapidly worsening muscle weakness.
© 2026 Rheumatology Care Associates. All rights reserved.